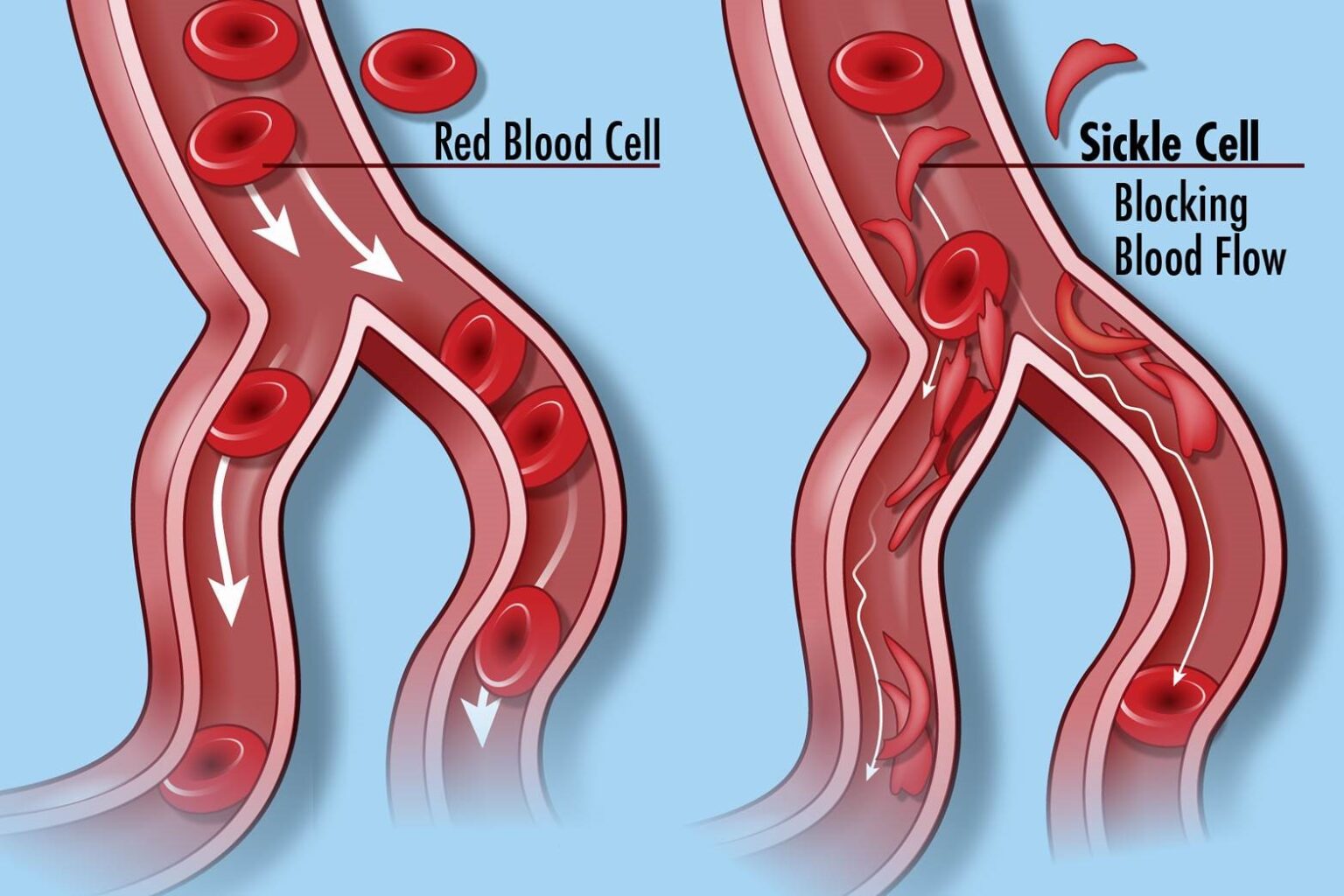
Vanderbilt University Medical Center is part of a 6-year, $4.4 million grant from the National Institutes of Health to improve the use of prescribed medication by sickle cell patients.
Funded by the National Heart, Lung and Blood Institute (Grant No. 1U01HL133996-01), the new Sickle Cell Disease Implementation Program includes researchers from St. Jude Children’s Research Hospital, the University of Memphis, Methodist University Hospital, Baptist Memorial Hospital and Vanderbilt.
The team will jointly develop, assess and integrate mobile health applications to manage hydroxyurea treatments among patients with sickle cell disease and identify barriers to medical care and any constraints on proper use of the medication.
In addition, the team will also make the findings of the study available nationwide to encourage best practice and wider use of hydroxyurea in the national sickle cell community.
The team from Vanderbilt, led by William Cooper, M.D., MPH, Cornelius Vanderbilt Professor of Pediatrics and Health Policy, will use administrative health care insurance data from Medicare, TennCare and a commercial payer to measure the use and impact of hydroxyurea for children and adults in the state.
Using this insurance data, the Vanderbilt team will identify Memphis-area patients with sickle cell disease and will then determine who among them has prescriptions for hydroxyurea.
The team will aim to identify potential focus areas for the other projects within the overall program, which is designed to intervene and improve prescribing the drug.
“We know that hydroxyurea is an important part of the care for sickle cell disease. Unfortunately, not every person who should be taking the drug takes it regularly,” Cooper said.
“This work will allow us to identify groups who may be helped by the intervention work that our collaborators here at Vanderbilt and St. Jude are planning.”
Hydroxyurea can greatly reduce some of the complications of sickle cell disease, but some studies have shown that only 15-35 percent of sickle cell patients adequately follow their prescribed medication schedules.
In the United States, more than 100,000 people are affected by sickle cell disease, mostly African-Americans and many from disadvantaged backgrounds. In the Mid-South region alone, sickle cell disease affects approximately 2,000 individuals. If not treated effectively, sickle cell disease can lead to organ failure and early death.
“While we have made good progress using hydroxyurea to help children and younger adults look after their disease, much remains to be done to slow the progress of sickle cell as older teenagers transition to adult life,” said Jane Hankins, M.D., an associate member of the St. Jude Department of Hematology and principal investigator of the project.
“Our goal with this project is to use mobile health applications to help 15-year-old and older patients in the Memphis and wider areas manage sickle cell. This is crucial since at this time in their lives they often have less access to health care providers and comprehensive sickle cell programs, which greatly impacts their quality of life.”
A research team led by Lisa Klesges, Ph.D., of the University of Memphis, will develop the app and measure the population impact of its implementation.
“We have assembled a multidisciplinary team of statisticians, epidemiologists and informaticians who will involve patients in the design of the new app and work closely with all collaborators to optimize the design and measure its use within the community system of care,” Klesges said.
Patients will be recruited and participate at four clinical centers — St. Jude, Methodist University Hospital, Baptist Memorial Hospital, and from a small private practice in Memphis.
The team will measure the impact of the program and collect all of the data needed to assess the effectiveness of the app.
The goal is to look at how many patients have adopted the technology and assess its reach, cost effectiveness and longer-term sustainability.
The desired outcome is to share the findings nationwide to make sure that sickle cell patients in this vulnerable age group have the best possible access to the most effective drug treatments.