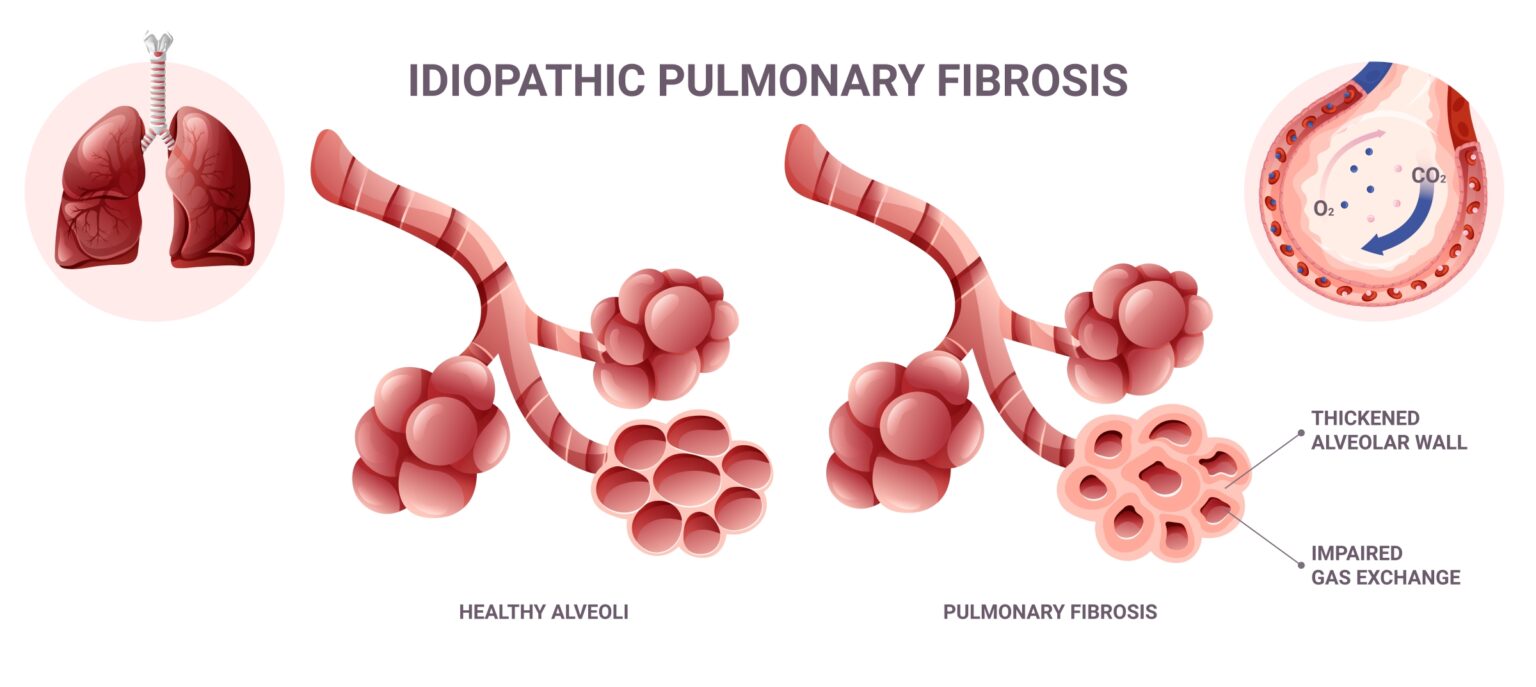
The standard treatment for idiopathic pulmonary fibrosis (IPF) that has been widely used for the last 20 years is not only ineffective, but appears to be dangerous, according to the findings of a clinical trial.
As a result, the National Heart, Lung, and Blood Institute (NHLBI), part of the National Institutes of Health, has stopped one arm of the clinical trial known as PANTHER-IPF that was studying treatments for the disease at Vanderbilt University Medical Center and two dozen other sites around the country that are part of the IPF Clinical Research Network.
The trial found that a currently used triple-drug therapy consisting of prednisone, azathioprine and N-acetylcysteine (NAC) is a potentially harmful combination to people with IPF. The study was designed to evaluate if this commonly used regimen could slow disease progression and improve lung function in people with moderate IPF, which is a progressive and currently incurable disease characterized by the buildup of fibrous scar tissue within the lungs.
“This is a landmark change in treatment because it shows that a treatment that has been used widely in the U.S. and around the world does not work,” said James Loyd, professor of medicine and Vanderbilt’s principal investigator for PANTHER-IPF. “It’s important to a lot of patients who have been prescribed this treatment as standard therapy. [rquote]If this treatment strategy is not effective, the sooner we know that, the better, and this trial is the first solid evidence.[/rquote]”
The study data showed that compared to placebo, those assigned to triple therapy had greater mortality (11 percent vs. 1 percent), more hospitalizations (29 percent vs. 8 percent), and more serious adverse events (31 percent vs. 9 percent) and also had no improvement in lung function tests. In addition, participants randomly assigned to the triple therapy arm remained on their assigned treatment at a much lower rate (78 percent vs. 98 percent).
In stopping this part of the trial, the NHLBI accepted the recommendation of the Data and Safety Monitoring Board (DSMB) – an independent advisory group of experts in lung disease, biostatistics, medical ethics and clinical trial design. The DSMB has been monitoring the study since it began.
“It’s very important that we learn from this and move forward,” Loyd said. “The only way to know in treating individual patients, outside of a controlled trial, whether a treatment is actually effective is for the disease to improve or disappear. For progressive diseases like IPF, that just doesn’t happen, so controlled trials are the only reliable measure.
“[lquote]The results of this arm of the PANTHER trial illustrate the critical need for multi-center placebo-controlled, randomized trials.[/lquote] Patient participation in trials is what has led to this important new information.”
Based on the results of the trial, Loyd recommends that IPF patients who are currently on this triple-drug therapy seek the advice of their physicians before stopping the treatment. Stopping prednisone treatment abruptly may cause serious health problems. It is important to note the combination drug therapy has not been shown to be dangerous for treating other diseases, such as connective tissue diseases, including rheumatoid arthritis, or for prevention of transplant rejection.
About 200,000 people in the United States have IPF, the cause of which remains unknown, and treatment options are limited.
PANTHER-IPF began enrollment in October 2009. The study had enrolled 238 of a planned 390 participants prior to the stop announcement.
The placebo and NAC arms will continue enrolling and following their participants, and this part of the PANTHER-IPF study is expected to be completed by late 2013.
Vanderbilt has a program of treatment trials for IPF, led by Lisa Lancaster, associate professor of pulmonology, assisted by four full-time research nurses. PANTHER is one of six IPF trials currently enrolling patients.