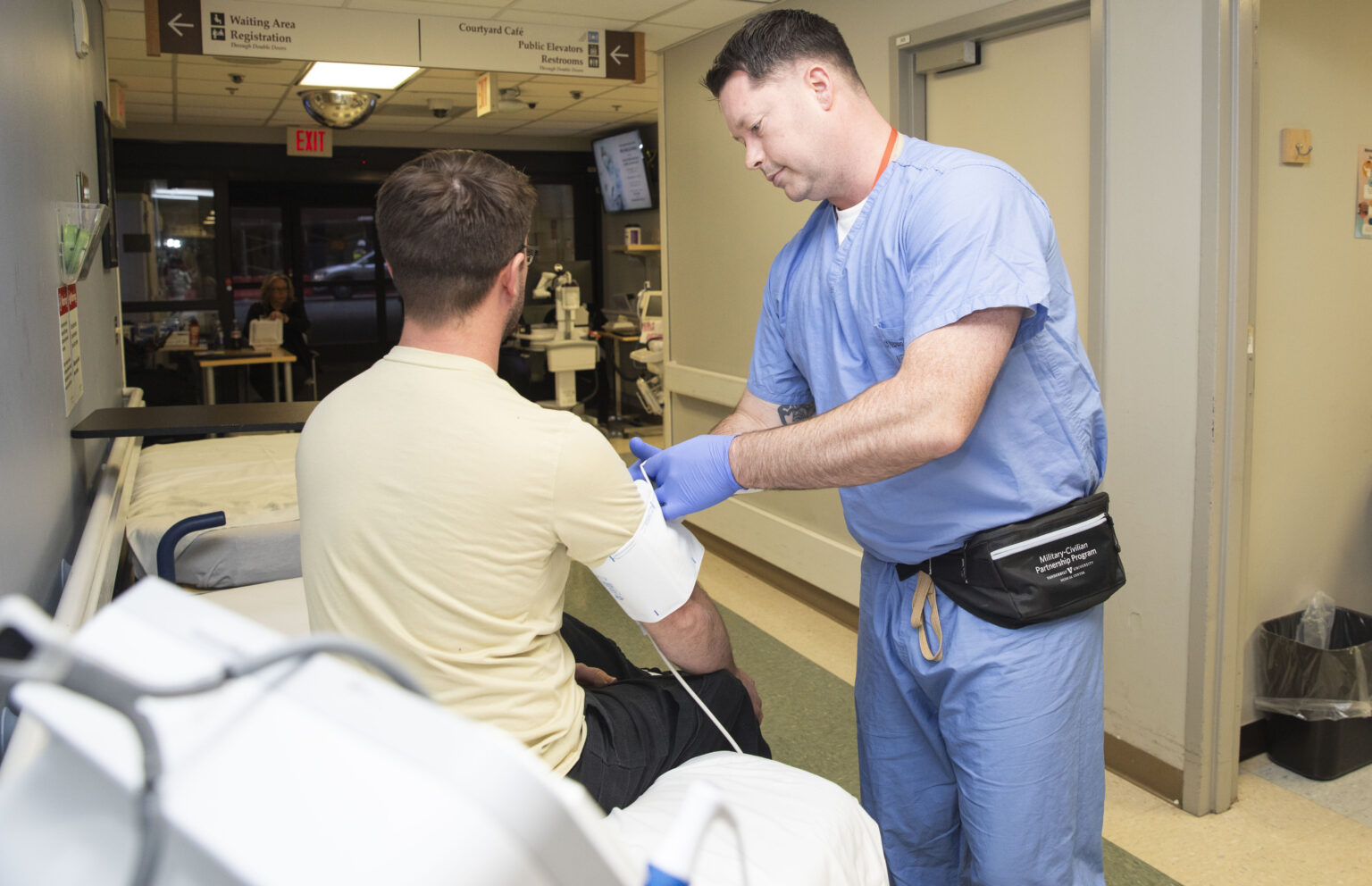
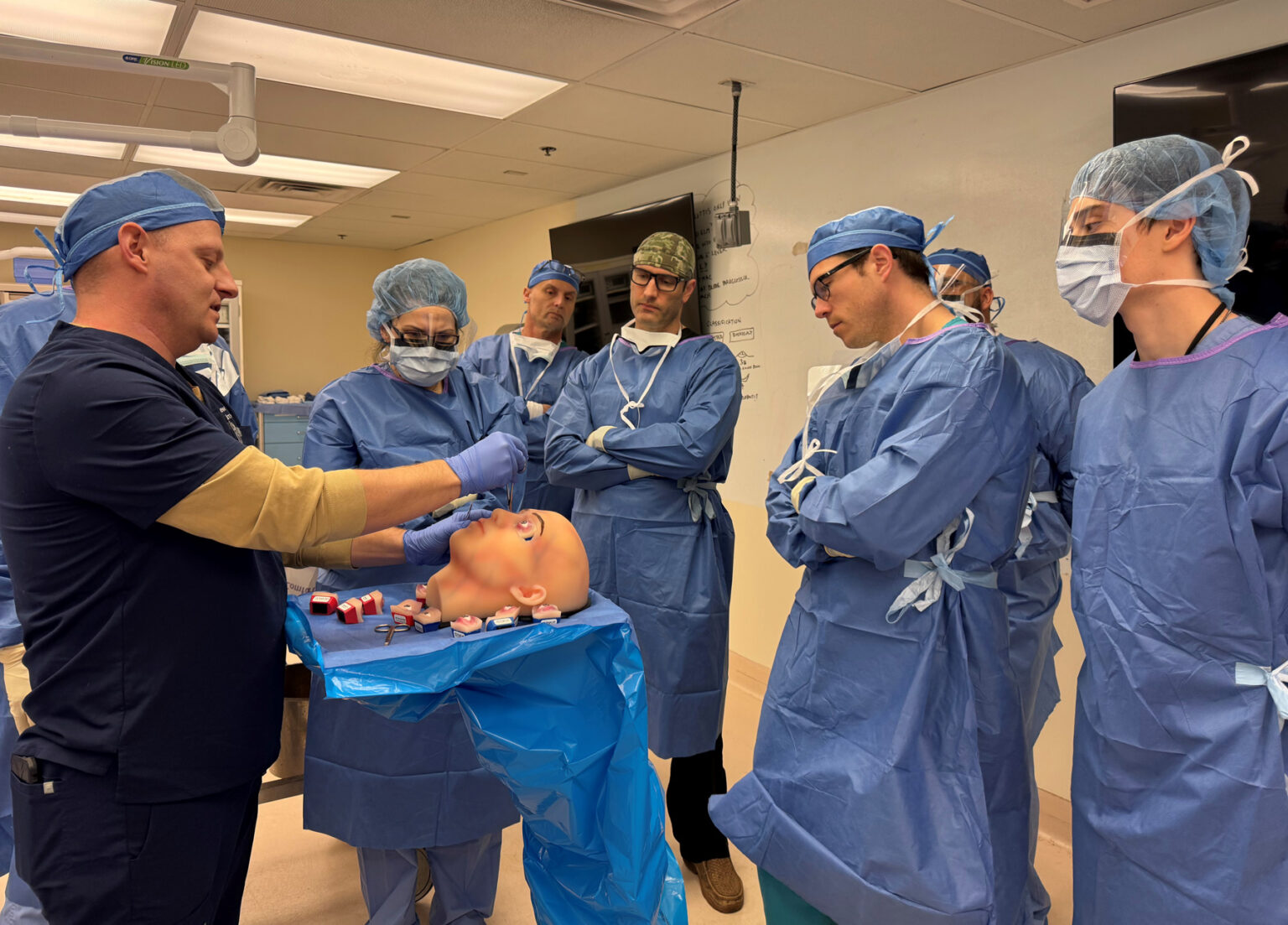
During a deployment as a military surgeon more than a decade ago, Vanderbilt University Medical Center’s Tim Nunez, M.D., felt ill prepared to perform complex trauma surgeries for an Iraqi family caught in a fire fight, but he’s now committed to helping military personnel become better trained for these types of emergencies.

“The first time I deployed to Iraq in 2003 was before I had done any specialized training,” said Nunez.
“At that time, I was a general surgeon doing routine general surgery cases — simple gall bladders and hernias on a relatively young, healthy, physically fit population. Then, I was in Baghdad. Totally different. We were taking care of people who had been shot and blown up. We were three general surgeons and an orthopedic surgeon, and we had all these traumas to take care of on one of our first days on the ground. I thought, ‘Oh, my gosh! What have I gotten myself into?’”
Nunez, who served more than 10 years as a U.S. Army surgeon, came to VUMC in 2007 to complete an acute care surgery fellowship. When he left the military in 2012, he returned to join the faculty as an associate professor of Surgery.
For several decades, VUMC and Blanchfield Army Community Hospital (BACH) at Fort Campbell have had informal exchanges in which military physicians, nurses, paramedics and techs come to VUMC for educational events and training, including rotations in the trauma and burn units. Likewise, VUMC physicians and other medical personnel travel to Fort Campbell to exchange knowledge with medical personnel there.
Now, as part of coursework toward a master’s degree, Nunez and a multidisciplinary team from VUMC and the Nashville Veterans Affairs Medical Center that includes two physicians, a nurse, social worker and financial planner, is developing a plan to strengthen the partnership with BACH, as well as with other military medical providers.

BACH Commander Col. Telita Crosland recently visited with R. Daniel Beauchamp, M.D., chair of the Section of Surgical Sciences, Seth Karp, M.D., chair of the Department of Surgery, and Nunez at VUMC to discuss this growing relationship.
“I am thrilled to know that we are extending and strengthening our long-standing relationship with Blanchfield Army Community Hospital,” said Beauchamp, also the John Clinton Foshee Distinguished Professor of Surgery. “We look forward to continuing our collaborative work with the medical professionals who serve in the military.”
Crosland said the partnership is invaluable in terms of building clinical skills for BACH personnel who typically don’t see high volumes of trauma and critical care as they work stateside, but added there are other ways in which the partnership is beneficial.
She is looking forward to consulting with VUMC as BACH works toward becoming a Level III Trauma Center, as certified by the American College of Surgeons (ACS).
“Another reason the partnership is important is due to a lot of exchanges of ideas,” Crosland said. “I don’t know how much it is publicized, but a lot of knowledge comes from military health back into the civilian sector. For example, with this last war, we’ve changed many things in terms of how trauma is managed because of the research the military has done with multi-amputees, resuscitation and other areas. When we partner with our civilian colleagues, we’re able to infuse that knowledge.”

Pampee Young, M.D., Ph.D., medical director of Transfusion Medicine at VUMC, traveled to Fort Campbell recently as part of an annual Education Day to speak about transfusion reaction and changes in blood-related products. Young has worked with BACH’s chief pathologists for a few years, sharing information on how to prepare for massive exsanguinations (blood loss events).
“Vanderbilt is a very large tertiary care/Level I Trauma Center and a large transplant facility with a comprehensive pediatric hospital as well,” Young said. “Our volume and breadth of services allows our large transfusion team to be exposed to unusual transfusion cases and also have access to emerging technologies. We can pass on that knowledge to military providers, who typically have a smaller scope of care and a smaller team of doctors involved with transfusion medicine.”
VUMC medical staff volunteer to take part in exchanges with BACH and other military medical groups, and it’s in addition to regular duties they already have at the Medical Center.
“When people ask why do we do this, I say ‘Because it’s our duty,’” Nunez said. “This is our military. We pay for every penny of it, so it’s our job to help take care of it.”
Crosland said she and her colleagues are appreciative of the continued support from VUMC through the years.
“When we went out to Vanderbilt, everyone was beyond gracious,” she said. “We know the community cares, and we know the community wants to support us. This is one of those clear, tangible ways that they are doing absolutely that. We are grateful for that passion and that patriotism.”