The following journal entries are written by Jay Wellons, M.D., chief of Pediatric Neurosurgery at Monroe Carell Jr. Children’s Hospital at Vanderbilt. In them, he recounts and reflects on Vanderbilt’s Fetal Surgery teams’ five-day trip to Australia to guide a team there through a historic moment.
7/19/2016: Nashville to Hong Kong
This is not the beginning of the trip. The beginning of the trip was back about 2 weeks ago when our Fetal Surgery team was asked to come to Brisbane, Australia, and help the newly formed fetal surgery team there perform two fetal operations and set up their program. The very next evening, because it’s a 15-hour time difference, the onslaught of paperwork began. Due to the diligent work of several of our administrative assistants (Thank you Debi), we are currently appropriately documented for a medical visit to Down Under and will be cleared, hopefully 2 hours after we arrive when we meet with the Australian Medical Board. It will have been a 25 hour trip. I hope they don’t judge us by our looks.
The group consists of seven individuals representing Vanderbilt: our leader is Kelly Bennett, Division Chief of Maternal Fetal Medicine in the Department of Ob/Gyn. Next, Stephane Braun from the Department of Plastic Surgery who is a critical member of the team (a major part of our “secret sauce” I like to say, to borrow a term from the VUMC President, Dr. Balser). Ray Paschall from the Department of Anesthesia, is here to “pass the gas” (not so easy considering that one of the two patients are usually safely behind the placental barrier). Ray has been involved with the fetal spina bifida effort since before the days of MOMS, aka The Management of Myelomeningocele Study. This landmark surgical, randomized trial was published in 2011 in the New England Journal of Medicine and convincingly showed that outcomes were better for infants operated on in utero versus after delivery. Vanderbilt was one of three centers chosen to be involved. The inclusion of Vanderbilt was due to the pioneering work by pediatric neurosurgeon Noel Tulipan in conjunction with Ob/Gyn Joseph Bruner. More on that later. Here at the airport, Ray regales us with a couple of stories of the old days and returns to his cellular phone, tending to his office duties before the flight. Ann Kavanaugh-McHugh, pediatric cardiologist, also a veteran of many fetal closure efforts, finishes up a phone call with her aging mother. Her role is to monitor the fetal heart filling and valve status during the operation. These are critical early signs of fetal distress that are seen by a trained eye and are important to the anesthesia and surgical teams in order to respond quickly. It is a great statement on the importance of each member of the team that Alicia Crum and Melissa “Missy” Broyles are here as well. Alicia does the vast majority of the fetal ultrasounds in the clinic, and all of them in the OR. Indeed she stands, scrubbed, directly to my left with a sterile ultrasound wand on the uterine wall and we often either bump elbows or entwine our arms so that we can do our jobs. It turns out that Alicia is the travel pro, having been to Tahiti and Istanbul over the years. This is by far the farthest that I have been away from home (did I actually want to be an astronaut when I was young?). Hearing her stories of travel calm the jitters of the long flight ahead. Missy, who works also in General Surgery and Urology in the Vanderbilt Main ORs is the scrub who is consistently involved with these operations, to the point that she has to be in town in order for us to schedule one of them. You may have heard of her type, intensely dedicated to her job, the team that she works with, and the patients that she serves. Hearing her take on what we go to do in a few days, clearly reminds us all of the purpose of our trip.
Carrying on Noel’s work
I view myself with two bad metaphors. (Technically one bad simile and one bad metaphor.) On occasion I feel like the Jack Swigert of the mission. For those not familiar with Apollo lore, Astronaut Jack Swigert was the Command Module pilot of the Apollo 13 mission, famously known as “NASA’s triumphant failure” when the oxygen tanks blew during a routine stirring causing an explosion that knocked a outer panel off of the Command Module, put the 3 astronauts in harm’s way, and started a saga that ended up with all 3 safely home. Swigert was called upon when the initial CM pilot, Ken Mattingly, was grounded for medical reasons one week before the launch. I am not anticipating a stir the tanks moment, and history showed that Swigert did his job and did it well, but in reality Noel really should be here. When other centers would either decline to teach others the procedure or charge a large fee to do so, Noel and the Vanderbilt group’s view was, “sure, come on down, and we’ll take you to dinner too.” It is critical to remember that every other center in the country completely shut down doing fetal neurosurgery for nearly a decade until the study was done. Hence, Vanderbilt’s ensuing attitude: “Maybe it is not our job to do each one of these, but maybe we can lead the field in interpreting the MOMS results and help to shape the future.” To Noel, he was simply “just closing the myelo here” when famously asked on a television special, focused on that one tiny patient as he continued his part in a revolution.
However, Noel is not here as he died too soon at 64 last year. Before he did, he asked me to help carry on his work through papers and education and doing the operations that came our way. So here I am. Headed over to the other side of the world, to operate for 20-45 minutes. That’s how long my part usually takes. If the lesion is large, then Dr. Braun and I will get creative with fetal flaps if need be. This leads to the second metaphor, that of the field goal kicker. There is so much time, energy, and effort by so many people to pull this off. All I need to do is come in the game, tap the holder, and put it through the uprights. I’ve done it time enough before. Noel did it more than anybody in the world. Neither of us, however, have done it in Australia.
7/21/2016: Arrival to Brisbane (2 days later)
Licensed to operate
Turns out that BNA (Nashville) to BNE (Brisbane) is a little more than changing a vowel. Once arriving in Hong Kong, our team was rerouted through Sydney, then on to Brisbane. With the time change and layovers and sleep deprivation, it was a little too calculus-like to calculate total travel time. We did barely make our meeting with the Australian Health Practitioner Regulation Agency. One of the highlights was seeing Ann, our seasoned pediatric cardiologist (and mother of 4 adult children), take out her original still-rolled-up diplomas and graduate school degrees and present them to the officials. “Hey,” she said as the official unrolled it like a scroll from the Queen herself, “I’d rather have pictures of my family in my office than these stuffy things. We have a pile in the attic for these.” This immediately made me re-evaluate all the stuffy things on my on office walls there to impress no one but me.
What we did find out is that the AHPRA is their version of the medical board, and that they had convened a special meeting out of session by conference call. We were told by the official representing us, that the response of the board was overwhelmingly positive, interested, and pleased that this was being brought to Australia. We also found out that the Mother’s Auxiliary through the Foundation at the Mater Mothers’ Hospital were the ones who raised the funds for our team to come — an incredible realization to hear that the already-mothers of the region believe in the well-being of the yet-to-be born children of their country. I look forward to meeting them and thanking the group in person.
7/22/2016: Simulation Day
It is hard to believe that it has only been just over 24 hours in Brisbane. This morning began at 8 a.m. with a simulation in the OR. There were more than 30 people involved and we performed every aspect of the simulation with all teams working together. We learned that Australians call their OR circulating nurses “Scouts” and that OR teams here are equally as interested in safety and culture as we are. There was a wonderful moment of chaos as the different teams (MFM, anesthesiology, scrub nurses, etc.) were issued separate colored scrub hats in order to identify each other better. We passed on our collective knowledge and experience to the team here over a 4-hour period as they better informed us of the culture specific to Australian operating rooms. Afterwards the Mater Hospital team had organized a symposium in which 3 of us gave presentations about the obstetric, neurosurgical, and anesthesia aspects of these procedures. This was well received by all. One of us took a selfie during the talk, in order to prove to his Chairman that we were indeed here.
Meeting the prospective patients: A difficult decision
Afterwards we screened the patients’ images in better detail and met the two prospective patients. There was a very difficult decision to recommend that only one of the two potential patients proceed with fetal surgery, due to the combination of neurosurgical and obstetrical risks taken together, and an unexpected finding on live ultrasound. An equally unexpected but critical aspect of this was for the Australian team to see how ours makes decisions together. Fetal myelomeningocele closure is the only fetal surgery for a non-lethal defect, so the reason to proceed needs to be clear, with less risk (including to both fetus and mother) than benefit (remembering that the benefit is to the fetus only), as best as can be estimated with the available data. One has to remind oneself that these types of procedures are already on the edge of risk, and it takes a judicious mind, silencing the external pressures, in order to best decide the path moving forward for each patient. There was a robust discussion back and forth in the team, and tears from the second prospective patient as it was clear it was not to be, but a good decision all around, based on experience and data.
Tomorrow we proceed with closure of a mid-level lesion in a fetus with normal-sized ventricles, an important predictor of those who would benefit from closure. The couple hails from well away from Brisbane, is highly informed, and felt comfortable with our final recommendation to proceed. Soon after, the teams were feted at a lovely reception with speeches by the hospital COO, the lead MFM of the Australian team, Dr. Glenn Gardener, and our team. (Thankfully, there were no selfies.) It’s clear of the collective pride that the administration, the doctors, the nurses, and the support staff all have in this happening at their institution, Mater. It was comforting to me to be in such a communal sense of well-meaning. It came, however, with the unfolding realization, that the eyes of the Australian medical community were beginning to turn towards Brisbane in anticipation for tomorrow morning.
7/23/2016: Operation Day
The day began early for everyone. Start time was 7 a.m., which meant that the OR staff, anesthesia team, and patient were all getting started hours earlier. The neurosurgery team, not so much. Dr. Martin Wood, Brisbane pediatric neurosurgeon, and I had struck up a quick friendship in the short 36 hours since our arrival, mostly over the shared life-experience of a busy neurosurgery practice, raising young children, having spouses that were also doctors, and managing our personal expectations for the operation to come. It was very important to me and to Kelly also that we not come in and just do the whole thing ourselves and go home. The concept of passing on surgical and medical decision-making is an interesting topic and one that is quite complex. A great deal of information can be transferred through conversations around a cup of coffee or a white board. Some certainly through simulations run or observation of surgery during collegial visits, but where the true passing of collective knowledge comes is in the merging of teams and the engagement of both in the procedure. This occurs time and time again during residency and fellowship training. Two colleagues working together and knowledge and information are passed along. We quietly spoke of critical steps and options that could be encountered, our surgical checklist, so to speak, in preparation for our part. Luckily, Martin could have had a second life as a barista lending itself to several cups of coffee over the preceding 36 hours, piccolos (a type of latte) the version of choice, but on the morning of surgery we could only stare at our clean cups until we were done. No tremors even slight, needed on this day.
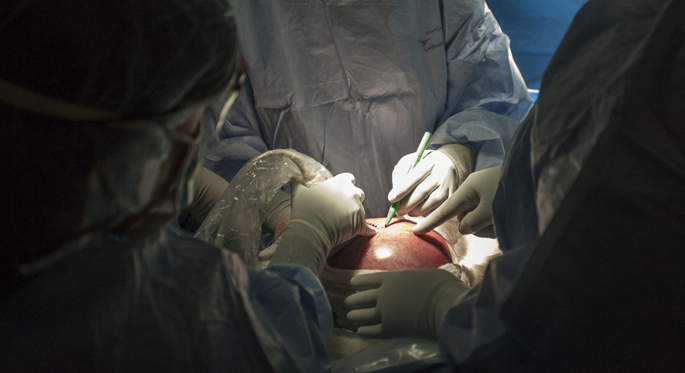
Dr. Bennett was paired off with Glenn Gardener, the lead Australian MFM. Glenn had the vision and determination to make this all happen. He and Kelly met years ago at an international meeting and he sequentially hatched a step-by-step plan to bring this procedure to the patients of Australia, first in conversation with U.S. counterparts, then observing the procedure at various institutions, then procuring the financial and institutional support necessary to bring an entire team over from the U.S. Their combined leadership was clearly evident throughout the entire effort, from the first surgical time-out and introduction of each and every team member at the prior day’s simulation to the positioning of the room and preparation of the patient’s abdomen. Each step, done together as teams, appeared to be starting smoothly. Ray worked with his Australian counterpart, Aldi, on appropriate IV lines and his particular method of anesthetic induction and maintenance. Melissa arrived at 4:30 a.m. to set up the complex instrument trays with two of the local nurses, and watched over the sterility of the back table with the same zealousness that we were used to at home. As the uterus was exposed, Alicia skillfully glided the sterile ultrasound probe over the pink dome, transmitting a healthy fetus and heart images to Ann, set up with line-of-sight in the corner. Kelly and Glenn worked through the uterine opening, minimizing damage to the muscle, and quickly sewing the placental membranes up to the inner wall when identified. This technique, developed by Kelly since MOMS, is one of the major reasons why we are here. A major drawback to intrauterine surgery is preterm birth. This exposes the neonate to several potential complications (mainly those of the lungs, gastrointestinal system, and cerebral cortex) that are avoided the closer birth comes to term. By this meticulous stitching and use of the stapler to keep the membranes from sagging away from the inside of the uterus, the likelihood of membrane rupture, loss of fluid, and triggers for earlier birth are significantly reduced. This was shown in a well-regarded paper published in Journal of Neurosurgery, Pediatrics in 2014 by our team. Here, the technique is on full show, and with the crack of the firing of the stapler, I turn to Martin, “Its time.”
“The clock is ticking, boys”
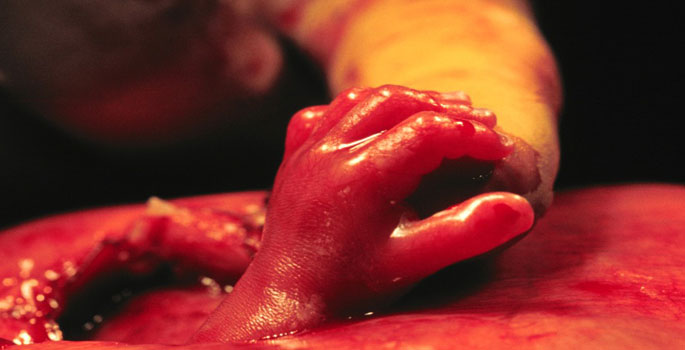
The room is quiet as we enter, hands up, palms in, fingers extended. We both wear surgical loupes and portable headlights in order to magnify and illuminate the area that we to operate on. Often as neurosurgeons we will use an operating microscope for those reasons, enabling us to better see the intended anatomy and perform the delicate surgery required. These are marvelous devices but are large and unwieldy and have no place today. As we approach the table, the rhythmic tones of the mother’s heartbeat are turned down just so, enabling Ray, Aldi, and their anesthesia team to clue us in if necessary. It is an appreciated gesture that allows us to focus better on the task at hand. Dr. Bennett turns the baby in the womb, and the glistening lesion comes into view. The exposed spinal cord, the size of two grains of rice put together, is suspended on a bubble of thin translucent tissue containing the spinal fluid. Martin and I quickly begin to dissect the tiny spinal cord and nerve roots from around the surrounding abnormal tissue. “The base is wide,” I remark as Martin works. “Stephane, we will be swinging flaps.” The base of the lesion is wide when compared to the normal skin. Gentle dissection of the normal fetal skin lateral to the defect typically allows us to bring the midline together and cover the neural tissue with normal skin. Here, however, the base is too far apart to do that. Alicia and I suspected as much from her ultrasound the day prior, and this confirmation then triggers another reason why we are here, the teamwork needed to perform bipedicled flap coverage on a 24-week-old fetus with a blood volume of 50 cc’s. Our team will soon be reporting our results with this technique, showing the same degree of success than when faced with the less complex fetal closure. Stephane and I work quickly. Kelly gently, but in her unyielding tone, reminds us of the fragile surrounding fetal membranes and nearby placenta, “The clock is ticking, boys.” The space in which we work is around the size of a tablespoon. There is a moment when Ann’s voice rings out, the heart is underfilling and the cardiac output drops slightly as the heart rate rises, an early sign of fetal stress. The room freezes, teetering on an edge familiar to seven of us alone, but in our tablespoon we carry on. This passes. Martin and I close the midline defect. It is his hands now bringing the midline together. “Let the record show,” I say. “The first fetal myelomeningocele closed on Australian soil was by an Australian doctor.” Stephane and I then quickly sew grafts into place along the fetal flanks, hands moving together, and we are done—42 minutes and 30 seconds, and Martin and I are swept over as the MFM team begins the uterine closure. It is, as they say in Brisbane, time for a coffee.
The debrief occurs among each team: anesthesia to anesthesia, MFM to MFM, and so forth. Over the next few hours, our patient awakens, speaks to her husband, and it’s clear that the deed has been done. A collective sense of relief turns to a wash of pride. Pride in a job well done for our Australian colleagues, pride in a hospital, auxiliary, and community fully invested, and pride in each other that such an amazing thing full of so many details can occur successfully. I will not deny that the feeling after a successful surgical endeavor outstrips any nearly every other emotional intensity. It is a strong wonder that I have on occasion felt in the family consultation room outside of the OR sharing the results to relieved parents but most often in the still quiet space of the changing room late in the day. Here, on the other side of the world, with people who we had truly never known until only a few days before, it was powerful and it was joyous and it was well-earned.
7/24/2016: Homeward Bound
There was an excellent Australian Rules Football game later that day, then a relaxed dinner. The next morning a press conference was called during which all of the major news networks appeared. Much focused on the first such operation in Australia, and then on the risk. Journalists do like risk and that is not in short supply in fetal surgery, but as the story grew over the next several hours, and the journalists realized what they truly had in this narrative, it became less about the sensational and more focused where it should, on the patients, on the teams, both Mater and Vanderbilt together, and on children with spina bifida and what can be done to lessen their burden.
As I reflect on this amazing journey, I cannot help but be struck by the kindness we encountered all around us. From the father, quietly watching the press conference, smoothing Glenn’s collar before we walked out to our seats, to the many faces at Mater Maternal Hospital in Brisbane welcoming us and ensuring that we had what was needed for the work ahead, or to Leigh-Ann, shepherding us through our days and nights (and ensuring that we hugged at least one Koala and tasted Vegemite in our 80 hours there). The story is certainly about a mother and a father, willing to accept risk, yes even death, just for the chance to help their unborn child live a better life. It is about a team willing to travel to the other side of the world, the team that brought them there, and the incredible willingness to share collective wisdom and jettison self-interest in order to help one amazing little family and in doing so make Australian history. Mostly, though, it is about what we are able to do together when we use our grit and our smarts to dream and do things much greater than who we are individually. As I sip my coffee and consider the last few days on the long flight home, I wonder what Noel would be thinking now. I wonder how he, a man of few words but much intention and ability, would have seen the great movements working around him and the significance of the events unfolding, all started years ago because he and a few others had a vision of how things could be for these children and families. I can hear his voice. “Just closing the myelo here.” Indeed Noel. Indeed.