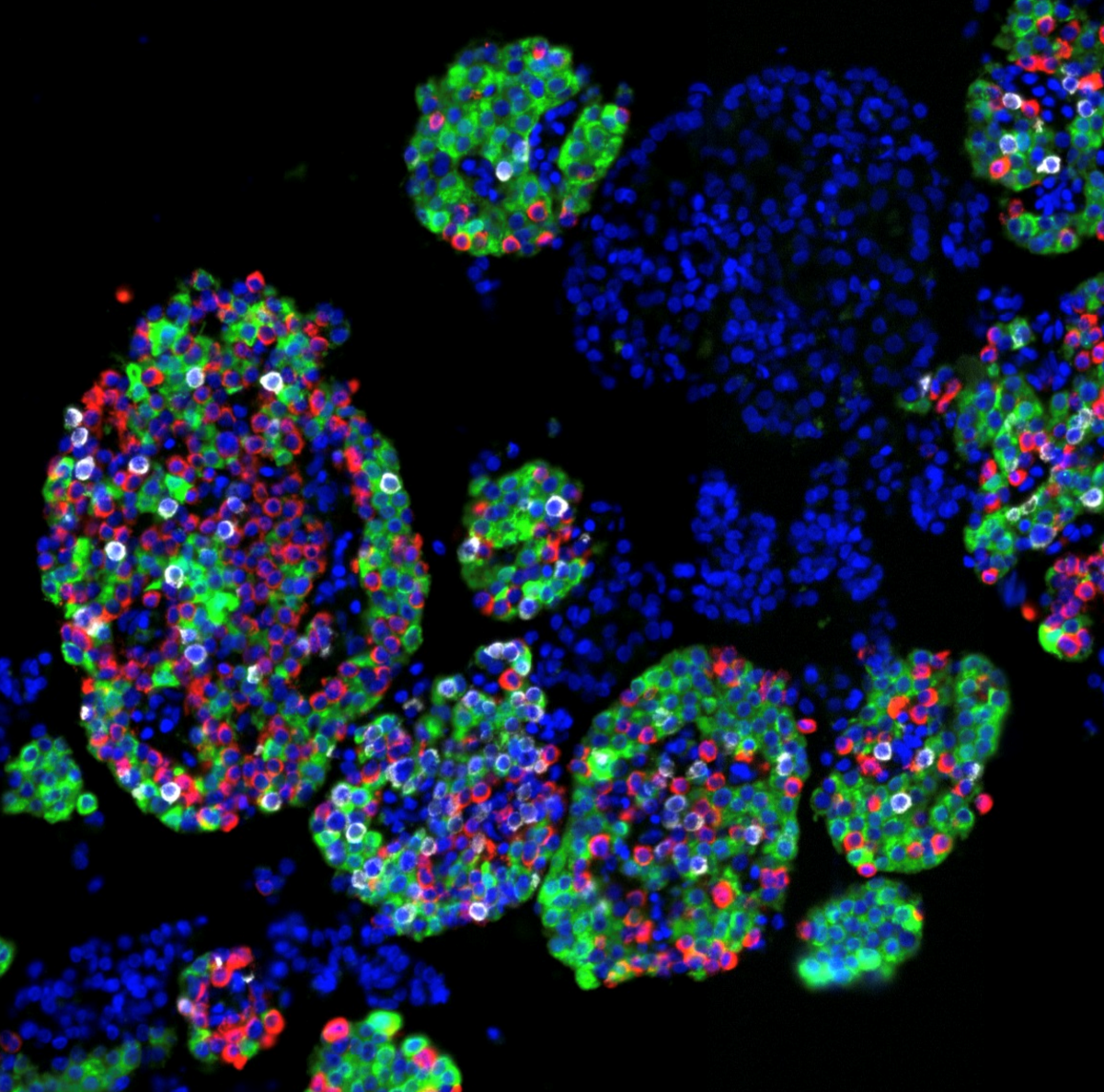
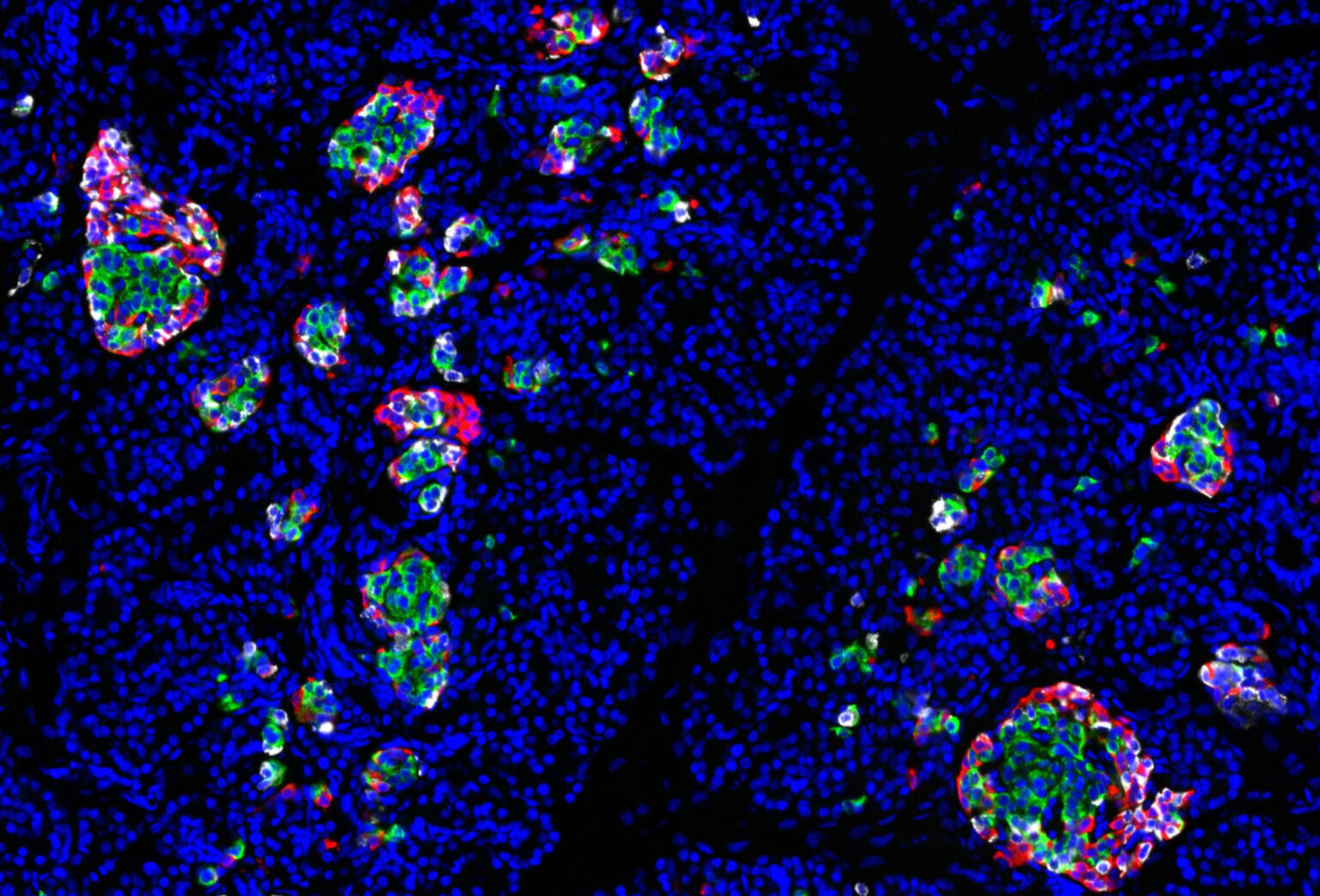
The use of human pancreatic islets to conduct diabetes-related research has greatly expanded in recent years, and a Human Islet Phenotyping Program (HIPP) at Vanderbilt University Medical Center has been established to provide important islet data to investigators worldwide.
In both type 1 and type 2 diabetes, the insulin-producing beta cells in the pancreatic islet are either destroyed or become dysfunctional, leading to insulin deficiency. In 2010, the National Institute of Diabetes, Digestive and Kidney Diseases (NIDDK) established the Integrated Islet Isolation Program (IIDP) that now works with five designated islet isolation centers in the United States to distribute high quality human islets to the diabetes research community to support scientific discoveries and translational medicine.
The IIDP currently supports 101 human islet studies in seven countries, and since its inception the program has distributed more than 112 million human islets to investigators, including a number of scientists at Vanderbilt.
As these studies using the human islet samples have progressed, investigators realized that there was great heterogeneity and variation in the characteristics of the islets being distributed. Because of this, the NIDDK, as part of the IIDP, sought to establish a national laboratory, the HIPP, that would analyze all of the human islet preparations that are distributed in order to record a phenotype or set of observable traits of the islets.
Vanderbilt Islet Procurement and Analysis Core Director Marcela Brissova, Ph.D., and her core laboratory were selected by peer review to establish the new NIH-funded HIPP. Vanderbilt’s selection is a direct result of foundational investigations that she and other Vanderbilt investigators have conducted in human islet biology, including studies emphasizing the importance of studying human islets, said Alvin Powers, M.D., Joe C. Davis Professor of Biomedical Science and director of the Vanderbilt Diabetes Research and Training Center (VDRTC).
“The establishment of the Human Islet Phenotyping Program builds on our long history of diabetes research at Vanderbilt, as well as Vanderbilt’s expertise and reputation in islet biology,” Powers said. “Now, every human islet preparation that is studied in the United States will be evaluated thoroughly by this Vanderbilt laboratory. Thus, the information obtained here at the HIPP will impact the diabetes-related research of more than 100 investigators at research institutions around the world by providing standardized, accurate information about the human islet samples.
“Human islet research has the ultimate goal of developing a cure for diabetes, and with the HIPP, Vanderbilt is positioned to continue to play a critical role in groundbreaking discoveries in this arena,” Powers said.
In July 2016, the first human islet samples were delivered to Brissova’s core laboratory for evaluation. To date, a total of 103 samples have been processed and evaluated by the HIPP.
“Our goal is to provide standardized assessment of islet phenotypes in terms of viability, function, composition, in order to better understand the relationship between these parameters and donor characteristics, for example body mass index, ethnicity and gender,” said Brissova. “An additional goal is to build a repository of human islet material that can be utilized by researchers.”
In December 2016, an IIDP HIPP database was developed, and this resource will soon be released online for use by subscribing researchers conducting research using human islets. As investigators in Brissova’s core lab analyze the human islet samples, they populate the database with key information about the samples. When investigators around the world receive human islet material from the same donor, they can log on to the database and access the data Brissova and her team have generated about that sample. This information will help guide and support the research of these scientists.
“We predict that the HIPP database will become a resource heavily utilized by the diabetes research community to advance understanding of islet biology and human islet function,” Brissova said.