The anonymous man being discussed in a conference room at Vanderbilt University Medical Center used to be healthy and athletic, but has suffered from slow progressive muscle weakness for some time and now uses a wheelchair to get around.
He is one of the thousands of patients looking for a diagnosis for something so rare they may never find the answer. But he’s one step closer today because of a weekly meeting of a dozen VUMC and Vanderbilt clinicians and scientists to discuss patients who have been accepted to the Undiagnosed Diseases Network (UDN).
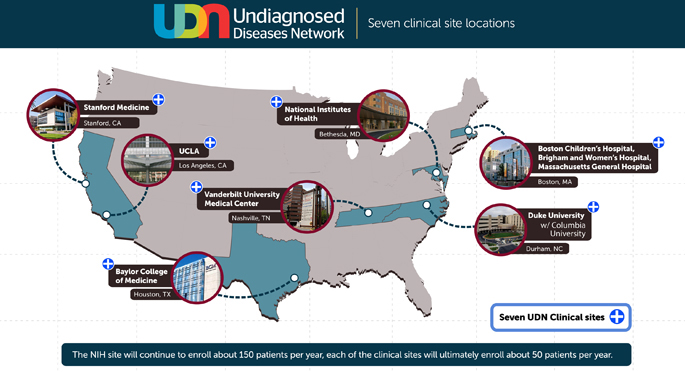
VUMC is one of seven sites around the country selected in 2014 to participate in a clinical research network to develop effective approaches for diagnosing hard-to-solve medical cases (undiagnosed diseases). The network’s purpose is to bring together clinical and research experts from across the United States to solve the most challenging medical mysteries using advanced technologies.
The UDN grew out of the success of the Undiagnosed Diseases Program at the NIH Clinical Center in Bethesda, Maryland. Since its 2015 launch, the UDN has reviewed more than 2,300 applications from patients around the world.
Through funding from the NIH Common Fund, seven hospitals and five core labs work together to try to solve medical mysteries through team science. At all seven sites, more than 1,000 patients have been enrolled for extensive genetic testing and a two- to five-day visit for a clinical evaluation.
Since September 2015, 317 applications have been referred to VUMC with 117 acceptances, resulting in 82 completed evaluations. Overall, about 30 percent of applicants are accepted. Those accepted consent to clinical testing, genomic sequencing as well as an extensive inpatient clinical evaluation, which, in many cases, can take five days. The patient’s DNA is analyzed either by whole exome or whole genome sequencing. To date, 51 diagnoses have been achieved through the Vanderbilt program.
The weekly meeting involves members of seven teams of scientists and data scientists from VUMC and Vanderbilt University. They come together to look at some of the analyzed data to see if they can trim a list of thousands of possible candidate genes to a shorter list of six to 15 candidates.
“It’s an agnostic kind of review with a goal of narrowing down the list of what genes could be causing the problem,” said Anna Bican, Vanderbilt’s site coordinator. “The goal is to determine if the patient has a new disease, an atypical presentation of a known disease or possibly two or more diseases. To do this, the group combines the patient’s medical history, in-depth analysis of DNA sequencing data, and additional input from the BioVU, GTEx and structural biology analyses. These diseases cannot be identified by genomic analysis or by an extensive medical evaluation alone. It is only in the pairing of the two together that the diagnosis can be made.”
The five groups represented at the weekly meeting are: VUMC-UDN group (presenting clinical data and data from three sequencing analysis pipelines); Department of Biostatistics; Center for Precision Medicine (phenotype risk scoring); Vanderbilt Center for Structural Biology; and Vanderbilt Genetics Institute (GTEx and PrediXcan).
“Every UDN site starts the review in the same way — with the initial lab report — but beyond that, each site goes about evaluating patients in a different way,” Bican said. “It’s important to have everyone in the same room. We start digging through the weeds and it’s all the minds in this group that bring us to a diagnosis.”
One team can look into BioVU to see if the particular genetic variants or others in the same gene have been seen in other Vanderbilt patients.
This helps eliminate variants that are too common to be causing a rare disease. Likewise, the GTEx/PrediXcan and structural biology teams also apply their methods to further narrow the list.
In this particular meeting, the group was excited about the possibility of a rare scientific phenomenon called “digenic disease.” This means that of the 23,000 genes in your body, of which only 3,900 are known to cause a disease, there are two defective genes that only in combination would cause a single disease.
The likelihood is rare. Typically, people would have two variants in one gene that causes disease. That’s called a compound heterozygote. Digenic is different because a person has two variants in two totally separate parts of their genome that together are causing illness.
According to the Digenic Diseases Database, there are only about 54 known digenic diseases. In fact, the whole field of study is relatively in its infancy, with the first case being discovered in 1994. With the advent of next-generation sequencing, the number of these digenic diseases is expected to grow.
“The goals of the UDN are to improve the level of diagnosis and care for patients with undiagnosed diseases and facilitate research into the mechanism of these diseases by creating a collaborative research community. The network also strives to better understand the impact of the diagnostic process on patients and families who have long awaited an answer,” said John Phillips III, MD, David Karzon Professor of Pediatrics, who is co-principal investigator of the Vanderbilt UDN with John Newman, MD, Elsa S. Hanigan Professor of Pulmonary Medicine, and Rizwan Hamid, MD, PhD, Dorothy Overall-Wells Professor of Pediatrics and director of the Division of Medical Genetics and Genomic Medicine at VUMC.
At the end of each visit, the UDN researchers share their findings in a meeting with the family to summarize the tests and procedures that were performed during the visit and determine what additional research may continue beyond the clinical evaluation, usually in a research laboratory.
Then a “wrap-up document” is sent to the patient’s referring provider since the UDN researchers can’t provide the permanent medical home for patients.
The document and what they learned during their UDN visit might identify improved options for optimal patient management, Bican said.
The success of the VUMC UDN site is driven by long-term institutional investment into resources such as BioVU, bioinformatics, precision medicine, structural biology and institutional support that has allowed the VUMC UDN site to tap into these resources.
“It is truly a campus-wide collaborative project,” Hamid said.