by Matt Batcheldor
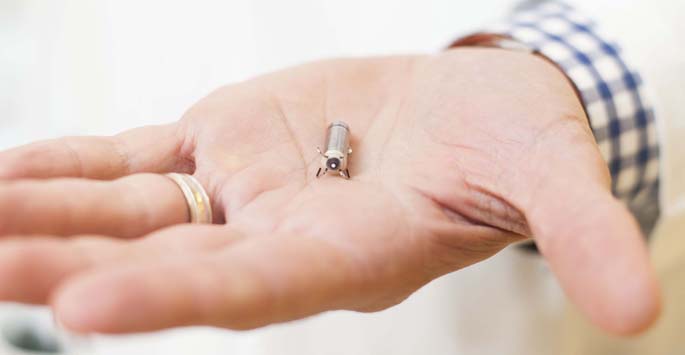
Martha Hawks remembers having the anesthesia mask placed on her face at the Vanderbilt Heart and Vascular Institute (VHVI). Next thing she knew, a pacemaker with wires that had been in her chest since 1996 was gone, replaced with the world’s smallest pacemaker, a wireless cylinder the size of a large vitamin.
In February, Hawks became the Southeast’s first recipient of the Medtronic Micra AV, the latest version of the tiny pacemaker that VHVI began testing in a clinical trial in 2014. The FDA approved the latest device in January.

Hawks, 70, of Glasgow, Kentucky, said she felt her old pacemaker every day for 23 years. But she doesn’t feel the Micra AV at all.
“I am just blessed, just blessed,” she said. “I feel really good.”
Installing the device, one-tenth the size of a conventional pacemaker, requires only a minimally invasive 35-minute surgery using a catheter inserted into a vein. Hawks’ procedure was more involved because her surgeon, Christopher Ellis, MD, associate professor of Medicine, also removed three pacemaker wires from the heart muscle and bone that had formed around them.
“This is definitely the first procedure in which an entire pacing system that had been in a patient for more than two decades was completely removed and replaced with a Micra AV,” Ellis said.
“That’s because we’re an experienced extraction center and have very good outcomes with that. You don’t necessarily take every single patient with a pacemaker and go laser out all the wires. But, in select circumstances, it’s probably a very appealing option.”
Attached to the heart via small tines, the Micra AV delivers electrical impulses that pace the heart through an electrode at the end of the device, eliminating the need for wires.
Unlike conventional pacemaker implant procedures, the new implant does not require a surgical incision in the chest and the creation of a “pocket” under the skin. It does not require a needle stick near the lungs either. This eliminates two potential sources of complications, and any visible sign of the device.

Pacemakers, the most common way to treat a slow or irregular heart rhythm, help restore the heart’s normal rhythm and relieve symptoms by sending electrical impulses to the heart to increase the heart rate.
Since the technology was founded about 50 years ago, pacemakers have largely looked and operated the same, Ellis said. Now that is changing.
The Micra AV expands access of the tiny pacemaker to about half of pacemaker patients in the United States. The earlier model, the Micra TPS, was appropriate for only about 15% of cases, best suited for patients needing a single chamber ventricular pacemaker. But the new model is able to treat patients with AV block, which occurs when the electrical signal coming from the upper chambers of the heart is blocked.
The new device has other benefits for Hawks. She has been a cancer survivor since 2008, but hasn’t been able to get an MRI because of her previous pacemaker’s wires. In December, she fell and hurt her shoulder and wasn’t able to get an MRI then. But now that the wires are gone, she can.
She did not hesitate to try the new technology. “I told him (Ellis) when you get ready to do this, would you give me the newest and the best? He said, ‘Martha, I’m just not sure it’s going to be available.’” It became available in the nick of time, around the time her old pacemaker’s battery was about to die. Her new one is expected to last at least 12 years.
“Dr. Ellis is just super good,” Hawks said. “The people (at VHVI) are just fantastic — nurses, doctors, technicians. Everybody that was involved was super, super nice.”