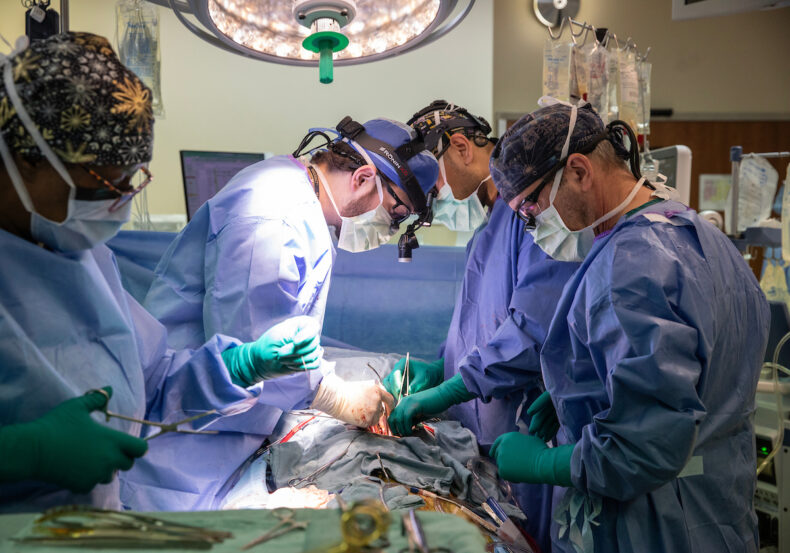
 Kascey Malone, CST; Aaron Williams, MD; Sean Bunch, RN; and Yatrik Patel, MD, work around a patient during a heart transplant surgery. (photo by Erin O. Smith)
Kascey Malone, CST; Aaron Williams, MD; Sean Bunch, RN; and Yatrik Patel, MD, work around a patient during a heart transplant surgery. (photo by Erin O. Smith)
Doctors have known that patients who have had a sternotomy prior to organ transplant are at increased risk after transplant. But that risk is not further increased by having more than one sternotomy, a study conducted at Vanderbilt Health found.
A sternotomy is a surgical procedure in which the breastbone (sternum) is divided down the middle to access the heart, lungs or other organs for major surgeries. Reoperative sternotomy is associated with increased use of blood products, risk of vasoplegia (severe low blood pressure) and posttransplant mortality, the paper states.
The paper, “Stacking Sternotomies: Does Surgical History Predict Post-Transplant Risk?” is published in the latest edition of the journal JHLT Open, a journal of the International Society for Heart and Lung Transplantation.
Researchers retrospectively reviewed 552 Vanderbilt Health patients from January 2024 to December 2025, placing them in three groups — those with no sternotomies, those with one, and those with two or more.
As in prior research, scientists found that one prior sternotomy increased risk but newly found that more than one did not add a statistically detectible additional risk.
“I think the reason this is important is I don’t think anyone has been able to study this with this size of a patient population and with the granularity of our analysis,” said corresponding author Brian Lima, MD, MBA, associate professor of Clinical Cardiac Surgery. “I think the results are really eye-opening and important to disseminate — not only to patients but to other centers — that maybe we need to rethink how we stratify risk when we are assessing patients for potential transplant who have had a prior sternotomy.”
Lima noted that this was a single-center study, and further studies are warranted to corroborate it with more data from other centers.
Lima said the reason patients are at higher risk after a major surgery involving a sternotomy is because, upon healing, they have developed scar tissue, which can bleed and make access difficult, making it more complex to perform further surgeries. But he added that higher-risk patients can be successfully transplanted, and the findings of the study could help doctors better understand risk.
“If you can really strategize and engage and approach it very systematically and methodically, you can make it a safe procedure, just obviously weighing the risks and benefits and educating the patients,” Lima said. “In my opinion, the benefits of a heart transplant far outweigh the risks in patients with heart failure.”
Ashish Shah, MD, professor and chair of Cardiac Surgery and a co-author of the paper, said the study highlights the power and size of Vanderbilt Health’s heart transplant program, the biggest in the world.
“As the world’s largest, we are able to ask and answer difficult questions with granularity and novel insights,” said Shah, who holds the Alfred Blalock Directorship in Cardiac Surgery. “Importantly, the study reflects our Vanderbilt Health approach: one that has been forged by hard lessons of the past, one with a modern emphasis on the best preoperative imaging and radiologist expertise combined with surgical experience. It all adds to our belief that historical risk can be mediated and patients given real hope.”
This research was supported by the National Institutes of Health (grants UL1TR000445 and T32GM007347) and the American Heart Association.






