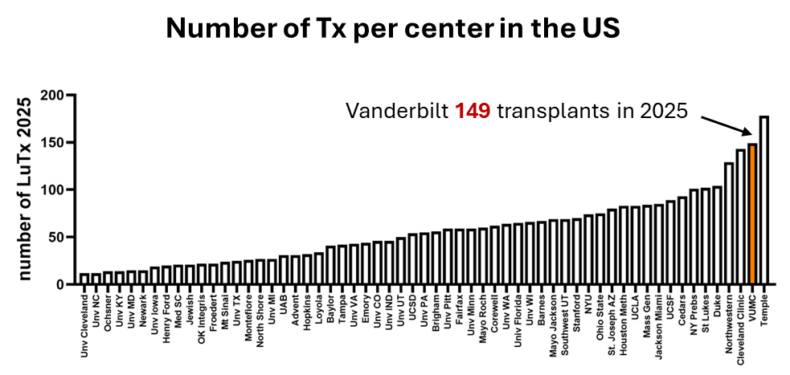
The Vanderbilt Transplant Center is now the second largest lung transplant center in the United States by volume, with 149 lung transplants in 2025, the most ever in one year at Vanderbilt Health.
The Vanderbilt Lung Transplant Program leads the nation in organ preservation and regeneration and is among the best in long-term outcomes, demonstrating the success of the interdisciplinary team in caring for these complex patients.
Several features make the program unique in the United States, said Konrad Hoetzenecker, MD, PhD, professor of Thoracic Surgery and surgical director of the Vanderbilt Lung Transplant Program. Vanderbilt serves as a “second opinion center” and accepts most complex candidates that are turned down by other centers due to increased perioperative risk.
This includes patients over 70 years old, patients requiring combined procedures with their transplant, multiorgan transplantations and sensitized patients (individuals who have pre-formed anti-HLA antibodies who are at higher risk for complications). The expertise and excellent outcomes have attracted patients far beyond the borders of Tennessee; almost half of Vanderbilt Health’s lung transplant recipients come from out of state.
“Another unique feature is our minimally invasive transplant program,” Hoetzenecker said. “By using distinct surgical instruments and techniques, the incisions can be kept as small as 7 to 8 centimeters, which results in better healing, less pain and faster recovery.
“This minimally invasive approach is embedded in an Enhanced Recovery After Surgery (ERAS) protocol, a multimodal, evidence-based perioperative care pathway designed to reduce surgical stress, minimize complications and speed up recovery. Our unique ERAS protocol, by a dedicated interdisciplinary approach, aims to improve recovery after lung transplant and reduce ICU and hospital stay.”
The lung transplant program recently celebrated a milestone — 1,000 lung transplants since the program began in 1990.
“This significant achievement reflects the concerted effort of a multidisciplinary collaboration by the Departments of Thoracic Surgery, Medicine, Anesthesiology and Critical Care,” said David Erasmus, MD, associate professor of Medicine and medical director of Vanderbilt Lung Transplant.
Lung transplants have been attempted since the 1960s, but they were largely unsuccessful until the 1980s, when surgical techniques were refined and new antirejection drugs proved effective. Patient outcomes steadily improved from the 1990s to the present. Vanderbilt’s fourth lung transplant recipient in 1990, Pam Everett, is the longest-living, single-lung transplant known in the world, recently celebrating 35 years since her transplant.
The Vanderbilt Lung Transplant surgical team is led by Hoetzenecker and Caitlin Demarest, MD, PhD, the surgical director and associate surgical director of the Vanderbilt Lung Transplant program. Erasmus is the medical director of Vanderbilt Lung Transplant along with Anil Trindade, MD, associate medical director and associate professor of Medicine.











