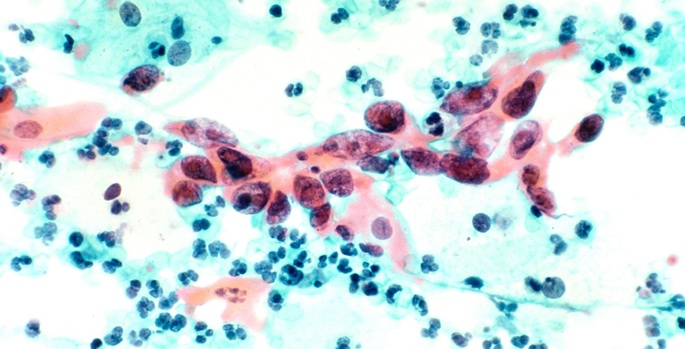
Douglas Lowy, M.D., acting director of the National Cancer Institute (NCI), warned that worldwide death rates from cervical cancer are expected to increase in low- and middle-income countries during the next 15 years unless steps are taken to prevent the cancer from occurring. Almost all cases of cervical cancer are linked to a viral infection.
Lowy made that prediction during his Vanderbilt-Ingram Cancer Center (VICC) George Daniel Brooks Lecture, delivered Jan. 24 at Vanderbilt University Medical Center (VUMC).

Jennifer Pietenpol, Ph.D., Executive Vice President for Research at VUMC and director of VICC, introduced Lowy as this year’s distinguished lecturer, saying, “The intent of the Brooks lectureship is to recognize investigators who have changed the face of cancer. There is no one more deserving of this honor than Dr. Doug Lowy. His research discoveries have changed the lives of tens of thousands of people and will have a positive impact on many more in the future.”
Lowy is chief of the intramural Laboratory of Cellular Oncology in the Center for Cancer Research at the NCI and specializes in research on papillomaviruses.
He and research collaborator John Schiller’s laboratory were involved in the initial development, characterization and clinical testing of the virus-like particle-based human papillomavirus (HPV) vaccines that have been approved by the FDA and many other countries.
Lowy said infectious agents, including the human papillomavirus, cause 15 to 18 percent of all cancers worldwide. HPV causes cervical cancer in women and other types of cancer among men and women, including oropharyngeal cancers of the throat and the soft palate, the base of the tongue, and the tonsils. Lowy noted these HPV-associated cancers, especially oropharyngeal cancers, “have been increasing substantially in recent years.”
Physicians at VICC have documented a large increase in HPV-associated cancers in the past few years.
HPV is a sexually transmitted virus that is extremely common. In most people the virus is shed and doesn’t cause any lasting issues. But in some patients the virus can trigger cancers that are lethal if not caught and treated early.
Three vaccines are approved by the FDA to prevent HPV infection. All three prevent infections with HPV types 16 and 18, two high-risk HPVs that cause about 70 percent of cervical cancers and a higher percentage of other HPV-associated cancers. Vaccination is approved for boys and girls as early as age 9 because the vaccines are designed to prevent infection and are not curative once a patient is infected.
Lowy said studies have indicated that the body’s immune response is stronger in patients under age 15 than patients who receive the vaccine in their late teens.
“In uninfected patients, use of the HPV vaccine can confer close to 100 percent protection against persistent infection and disease attributable to HPV vaccine types,” he said.
But he noted that prevention is an area that tends to be neglected. While there was an initial rise in the use of HPV vaccines in the U.S., vaccination rates appear to have plateaued and some parts of the country, including Tennessee, have very low vaccination rates.