 Newborn Annie, listed by her first name, Helen, on her bassinette, rests after the emergency delivery that prompted rapid intervention from Vanderbilt Clarksville Hospital’s labor and NICU teams. (courtesy/Ariel Chavis)
Newborn Annie, listed by her first name, Helen, on her bassinette, rests after the emergency delivery that prompted rapid intervention from Vanderbilt Clarksville Hospital’s labor and NICU teams. (courtesy/Ariel Chavis)

Ariel Chavis knows she didn’t get preferential treatment from the Vanderbilt Health obstetrics and labor and delivery teams when she gave birth last July. After all, it wasn’t until after she’d delivered her daughter that the doctors and nurses who saved her life, and her baby, caught on to the fact that she worked in another unit of the hospital, now called Vanderbilt Clarksville Hospital.
But, as you would expect for someone who had a brush with death and made it out with a healthy baby, it sure felt to Chavis like she received care from people who thought she and her now 7-month-old daughter, Helen (affectionately known by her middle name, Annie), were the most important people in the world.
The ‘nurse curse’ looms
Chavis, now a mother of two, was no stranger to pregnancy complications. After undergoing an emergency cesarean section when she gave birth to her first child in 2023, she entertained the idea that the “nurse curse,” which posits that whatever can go wrong will go wrong for nurses receiving medical care, might have struck her.
But that first regular C-section was a walk in the proverbial park compared to the difficulties Chavis faced when Annie arrived.
Chavis, at 41 weeks pregnant, was on high alert for anything that seemed off about the final stages of her term — and something felt abnormal. She and her husband, Jeremy, made their way to the hospital, where Vanderbilt Health has supplied pediatric neonatologists for the hospital’s Level II neonatal intensive care unit (NICU) and nursery for years.
When Chavis arrived, she felt right at home in the hospital where she spends her working days. Once admitted and induced, things seemed to be progressing positively until pain struck her.

“It kept getting worse and finally came to a head when they turned me onto my left side, and I felt really dizzy,” said Chavis. She voiced her concern to a nurse. “Thankfully, she listened; she was watching; she was very concerned. The nurse-midwife came in, and I could just see the look on her face … something is wrong.”
The on-call physician agreed and told her care team she needed to go to the operating room immediately.
Minutes to save two lives
Chavis’ memory of the ensuing moments is hazy, but she eventually learned she endured two extremely uncommon childbirth complications: a uterine rupture and a complete placental abruption.
According to her care team, the odds of both happening to the same person during childbirth are around 1 in 5,000. One doctor estimated he’d seen a birth as complex as hers no more than three times in his 20-year career.
And in situations like this, every second is critical. According to a study in the “American Journal of Obstetrics and Gynecology,” performing a successful delivery in under 17 minutes when faced with these complications is highly likely to save the baby. Chavis’ surgical team delivered Annie in 14 minutes.
Complications continued after Annie arrived. At one point, Annie had been fully enveloped inside her mother’s abdominal cavity and had swallowed blood. When Chavis came to, her husband asked how she was doing, but she was preoccupied with the absence of crying. Annie wasn’t breathing.
“I said, ‘I don’t hear our baby crying,’” said Chavis. “He looked, and the amazing NICU team was already working on her.”
The nurse practitioner assured her Annie was in great hands and was off to the NICU and told her not to worry. With her breathing restored, Annie’s recovery began.
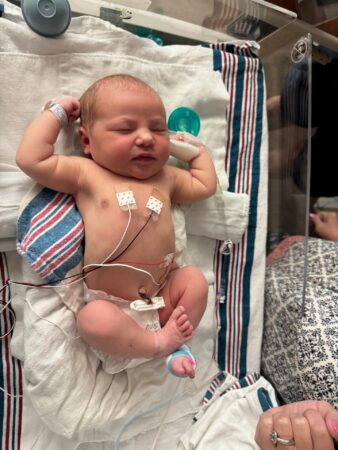
A fragile start, a strong finish
“The NICU team was absolutely phenomenal,” Chavis said. “They were on top of absolutely everything. We were very thankful to the team for working as hard as they did.”
Chavis said the NICU’s attending physician was initially so worried about Annie’s condition that he assumed she would be transferred to Monroe Carell Jr. Children’s Hospital at Vanderbilt in Nashville. Ultimately, he was so pleased with her recovery at the NICU in Clarksville that Annie got to remain close to home for the duration of her stay.
Chavis credits the doctors and nurses for doing their job with precision, adding that “it definitely counted not only for my life, but for my daughter’s life too. And that is why I have a little girl who is happy and healthy.”
Diane Attardi, MD, assistant professor of Clinical Pediatrics at Vanderbilt Health — who also serves as an attending neonatologist and the medical director of the Level II NICU in Clarksville — said the collaboration between Vanderbilt Health and local hospitals has sparked top-of-the-line care for patients like Chavis.

“Annie was in our NICU for four days and did great, and her recovery through the care of our neonatology team speaks to the success of Vanderbilt Health’s presence in Clarksville,” said Attardi. “This is a wonderful story and encompasses the expert care provided in three of our women’s and children’s units — Labor and Delivery, NICU and Mother-Baby — on our third floor.”
Attardi specifically lauded the nurses who supported Chavis’ recovery and who work tirelessly to ensure a seamless patient experience.
As a Clarksville resident, Chavis was excited when Vanderbilt Health partnered with Tennova, and is looking forward to the next chapter of working at the hospital now that the hospital is Vanderbilt Clarksville Hospital as of Feb. 2.
Speaking as both a patient and a member of the hospital staff, Chavis said, “I encourage anybody to deliver here because we have some of the best doctors and nursing care, especially on the third floor.”






