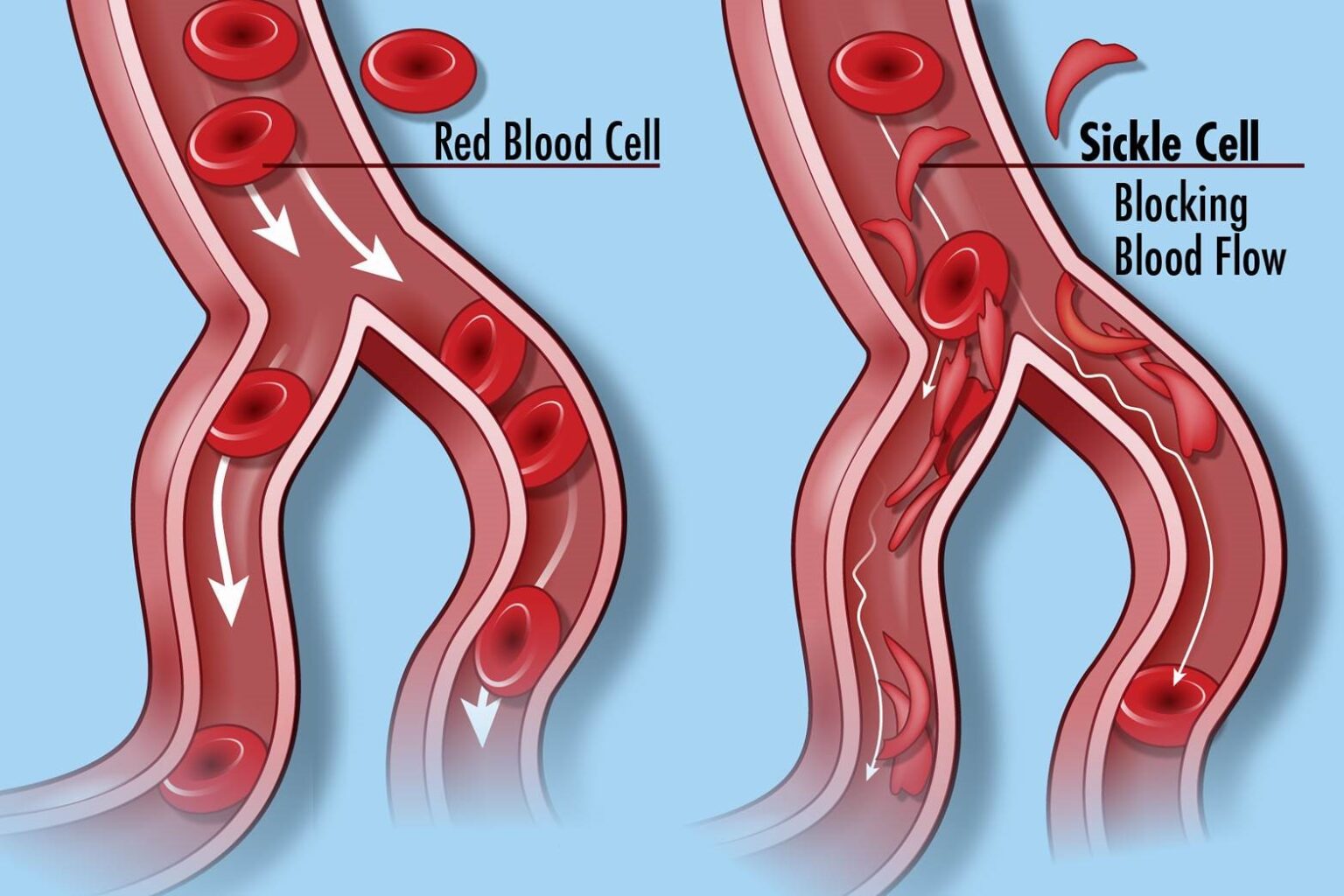
 Normal blood cells (left) and blood cells in sickle cell disease, which do not flow smoothly through the circulatory system. (image credit: Darryl Leja, NHGRI)
Normal blood cells (left) and blood cells in sickle cell disease, which do not flow smoothly through the circulatory system. (image credit: Darryl Leja, NHGRI)
Children with sickle cell disease are more likely than other children to develop a clonal growth of precancerous blood cells called clonal hematopoiesis (CH), which is associated in older people with a higher risk of blood cancer, according to new research from Vanderbilt Health.
However, the clones in children with sickle cell disease did not expand as readily as they do in older people with CH, suggesting that they may be more transitory and have different health consequences, the researchers reported March 26 in the journal Blood.
In addition, hydroxyurea, which reduces painful episodes and the need for blood transfusions in people with sickle cell disease, did not increase the risk of developing CH. That is good news for patients for whom hydroxyurea is “an essential therapy,” the researchers reported.
While questions remain about the link between CH and sickle cell disease, these findings shed light on disruptions in normal blood cell development (hematopoiesis) that may be shared by both diseases.
Chronic hematopoietic stress within the hypoxic (low oxygen), inflammatory bone marrow environment of sickle cell disease may predispose to the accumulation of somatic mutations (in nonreproductive cells) and/or the outgrowth of affected hematopoietic stem cell clones at an earlier age, the researchers hypothesized.
The researchers used a highly sensitive sequencing technique to determine the prevalence of CH in 1,025 children with sickle cell disease, and in a matched control group of 2,957 children without the disease. The results were validated in an independent cohort of 1,293 children with sickle cell disease.
Jessica Ulloa, a graduate student in the Vanderbilt Human Genetics Program, is the paper’s first author.
Contributing equally to the study were the paper’s corresponding author, Alexander Bick, MD, PhD, the Edward Claiborne Stahlman Professor and director of the Division of Genetic Medicine and Clinical Pharmacology at Vanderbilt Health; Michael DeBaun, MD, MPH, the J.C. Peterson, MD Professor of Pediatrics and director of the Vanderbilt-Meharry Sickle Cell Disease Center of Excellence; Santosh Saraf, MD, University of Illinois; and Mitchell Weiss, MD, PhD, St. Jude Children’s Research Hospital.
Other co-authors from Vanderbilt Health were Kristin Wuichet, PhD, Yash Pershad, and Connor Shore.
Support for the study was provided in part by National Institutes of Health grants R01HL168179, T32GM145734 and T32GM007347, and the Vanderbilt Undergraduate Summer Research Program.