lung cancer Archive — Page 1 of 8
-
December 2, 2025
Women who receive mammograms also undergo lung scans if notified of eligibility
Study showed that the improvement in lung cancer screenings exceeded the target enrollment set by the researchers. -
August 28, 2025
Genetic analysis of people with African ancestry reveals lung cancer susceptibilities
Prior research has shown that Americans of African ancestry have a higher risk of lung cancer compared to white Americans despite smoking fewer cigarettes, but the reasons for this difference are not fully understood. -
May 18, 2025
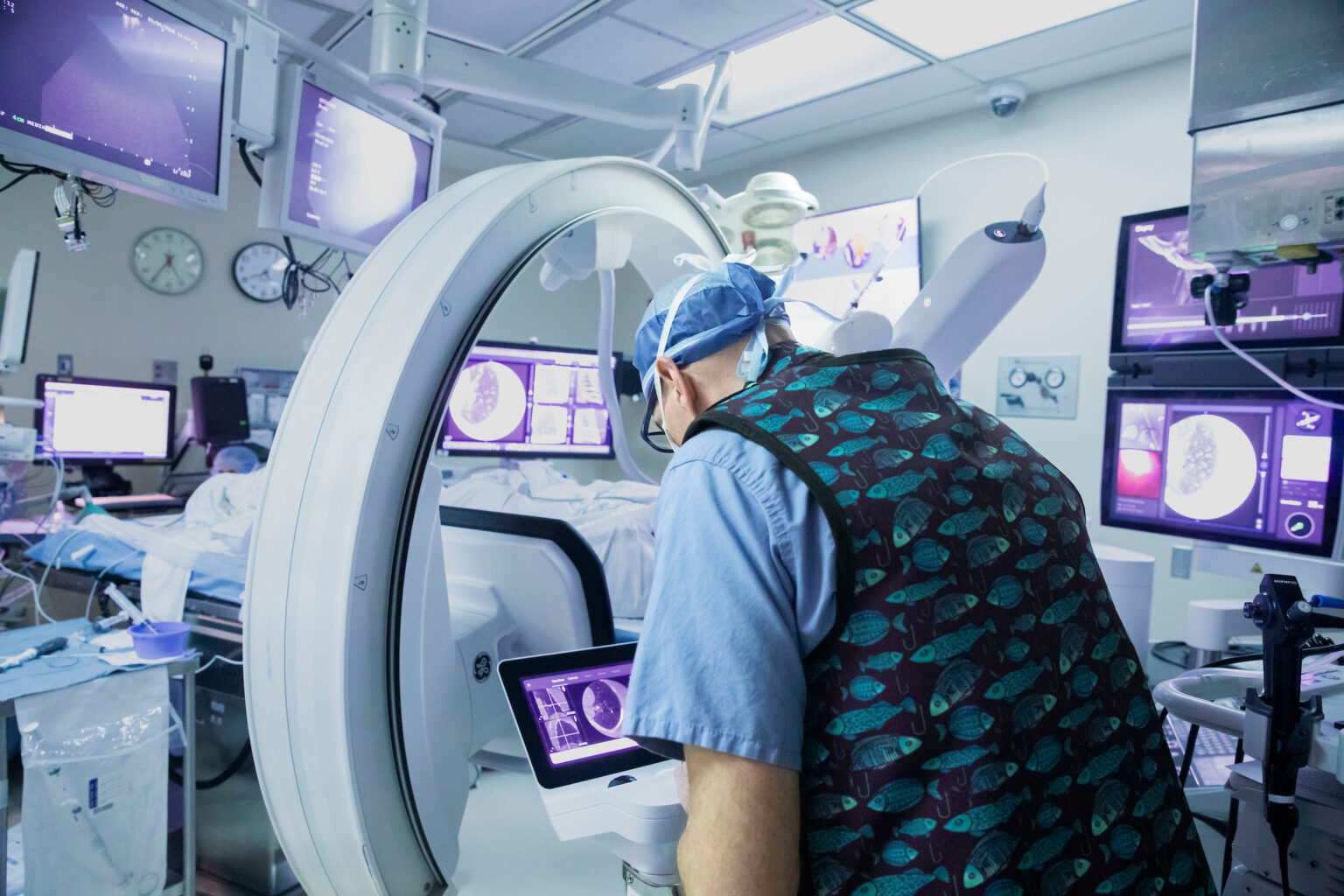
Study finds navigational bronchoscopy as effective and safer alternative to transthoracic biopsy for lung nodules
Each year, millions of lung nodules are detected during routine X-rays or CT scans. -
November 15, 2024
New radiation therapy approach for treating lung cancers
VUMC researchers tested a treatment combining immunotherapy and online adaptive radiotherapy, which is tailored to real-time tumor changes during the treatment plan. -
October 7, 2024
VUMC hosts International Lung Cancer Consortium meeting
The consortium is coordinated by the International Agency for Research on Cancer with the aim of sharing data from ongoing lung cancer case-control and cohort studies. -
September 20, 2024
Melinda Aldrich elected to genetics society board of directors
Aldrich uses population-based cohorts and biobanks to investigate lung cancer; her research informed guidelines for lung cancer screening. -
September 20, 2024
VUMC physician-scientists recognized for extending veterans’ lung cancer screening
Lucy Spalluto, MD, MPH, and Jennifer Lewis, MD, MS, MPH, are the recipients of the 2024 VAQS Team Award for work they began in 2017.