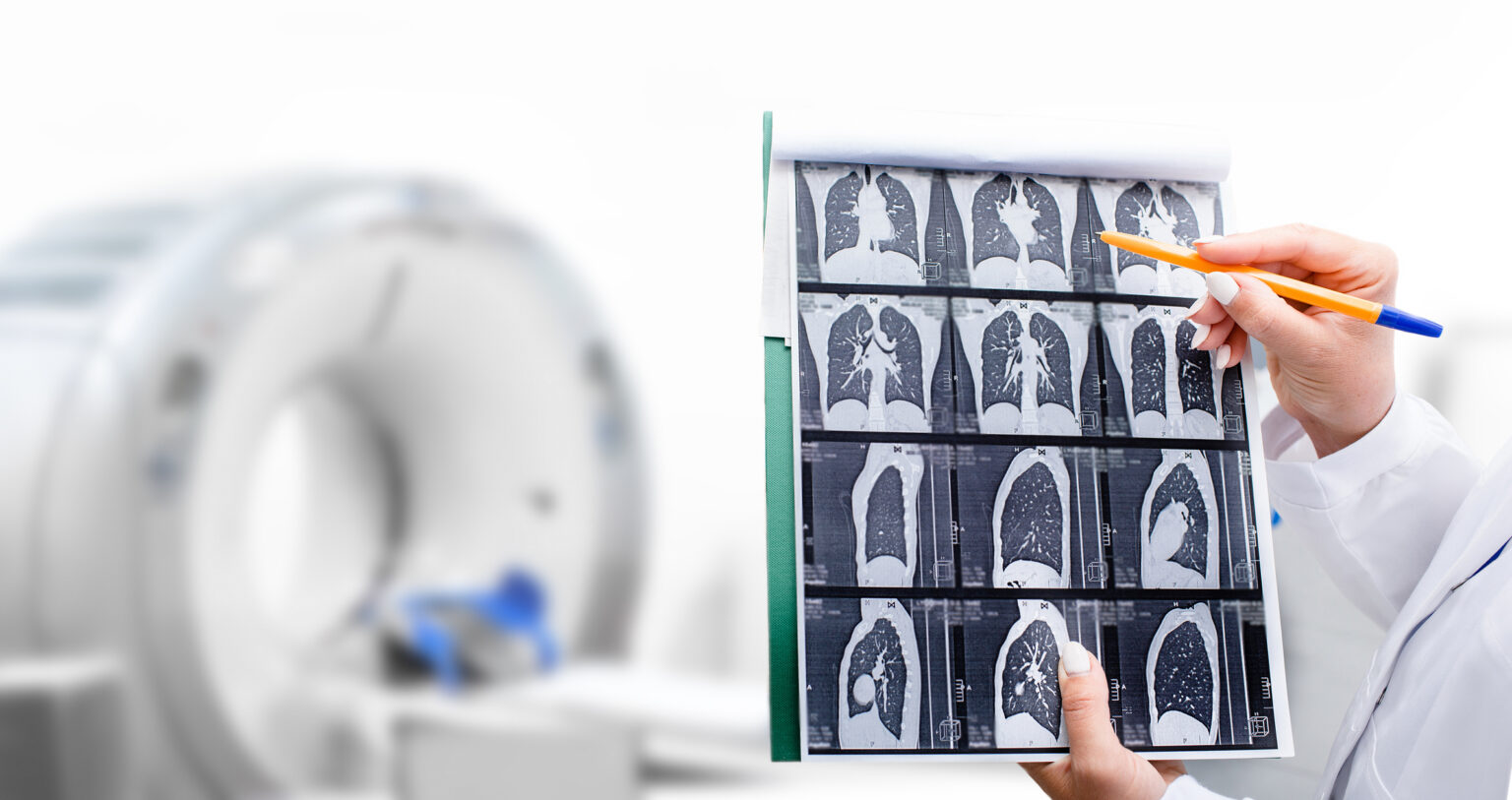
Lung screenings are an important diagnostic tool for early detection of cancer, but low-dose CT scans cannot determine whether the pulmonary nodules identified in the imaging are cancerous or benign.
Specially trained radiologists, pulmonologists and thoracic surgeons analyze the imaging and then decide whether invasive biopsies are warranted to make that determination — a process called risk stratification of indeterminate pulmonary nodules.
An estimated 10% to 15% of the resections of these nodules turn out to be surgeries for benign tissue. Risk prediction software using artificial intelligence, such as the Lung Cancer Prediction Score, which was developed by Optellum, a lung health technology company, and approved by the Food and Drug Administration in 2021, aids clinicians in determining whether surgical resections are necessary. In a recent study, Vanderbilt Health researchers determined that AI-assisted decision-making with this software is cost-effective compared to clinician assessment alone.
The study, published March 5 in PLOS ONE, showed that AI-assisted decision-making resulted in an incremental cost-effective ratio of $4,485 per life year gained.

“Artificial intelligence-based tools offer promising assistance to busy clinicians who evaluate suspicious lung nodules and seem to be cost-effective,” said the study’s corresponding author, Eric Grogan, MD, MPH, Ingram Professor of Cancer Research and professor of Thoracic Surgery at Vanderbilt Health.
To determine cost-effectiveness, the researchers constructed a decision model assuming guideline-based care from a payer perspective with a lifetime horizon. The base case is a 1.1 centimeter indeterminate pulmonary nodule in a 60-year-old patient who benefits from surgery. This nodule’s risk for lung cancer is about 65%. The model classified patients as low, medium or high risk using either clinician reasoning or clinician-plus-AI reasoning.

“When we think of these AI clinical decision aids, they may not really help the true clinical expert, the thoracic radiologist or pulmonologist who sees 20 of these a day. Where the larger health care system impact occurs is when generalist physicians can rely on these tools to remove the easy, cancer and not cancer cases, so they can focus or get a consult on the most difficult,” said the study’s senior author, Stephen Deppen, PhD, associate professor of Thoracic Surgery and co-director of the Early Detection Research Network Lung Group’s National Clinical Validation Center.
Other Vanderbilt Health authors are Caroline Godfrey, MD, MPH, Ashley Leech, PhD, MS, Kevin McGann, MD, Jinyi Zhu, PhD, MPH, Hannah Marmor, MD, MPH, Sophia Pena, Fabien Maldonado, MD, MSc, Evan Osmundson, MD, PhD, and Stacie Dusetzina, PhD. The researchers received support from National Institutes of Health grants T32CA106183, K01DA050740, R01CA253923, P30CA068485, U01CA152662, R01CA252964 and U01CA152662.