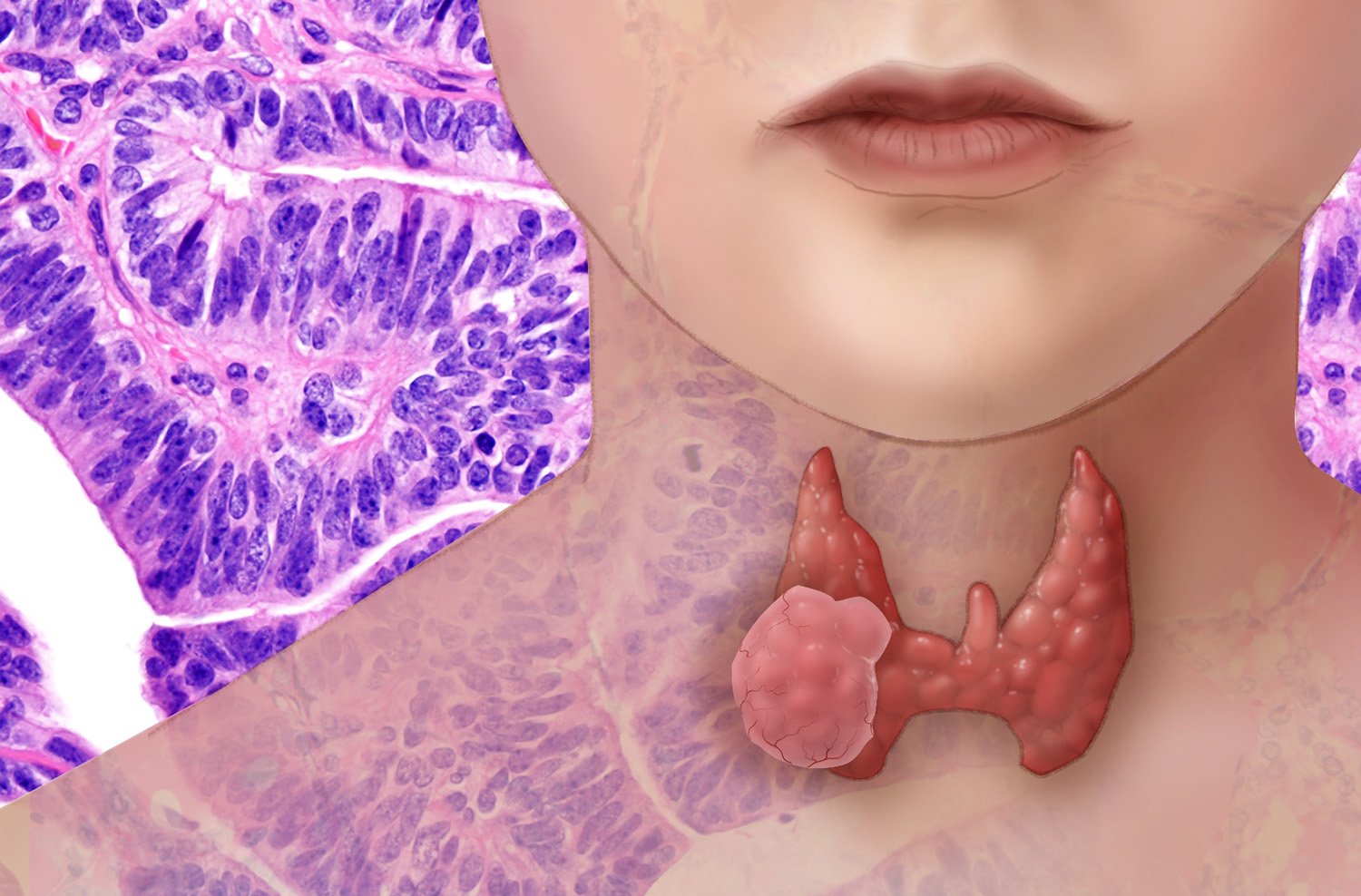
 While thyroid cancer is very treatable with surgery and other therapies, it remains the fastest growing cancer in the United States. (image courtesy of Darryl Leja, National Human Genome Research Institute)
While thyroid cancer is very treatable with surgery and other therapies, it remains the fastest growing cancer in the United States. (image courtesy of Darryl Leja, National Human Genome Research Institute)
A recent multi-institutional study led by physician-scientists at Vanderbilt Health found that there are certain types of stromal cells called fibroblasts that contribute to the invasion and progression of aggressive thyroid cancer. This work, published in the journal JCI Insight, defines the types of stromal cells (which make up certain types of connective tissue) present in thyroid tumors and identifies specific fibroblasts that appear to contribute to cancer cell invasion.
Understanding the danger posed by these cancer-associated fibroblasts (CAFs), which promote cancer growth, metastasis and treatment resistance, will allow for the development of targeted drugs to combat cancer in patients for whom surgical intervention was not effective.

The paper’s senior author, Vivian Weiss, MD, PhD, associate professor of Pathology, Microbiology and Immunology, credited the collaborative effort between numerous institutions for yielding results that show promise for the future of understanding thyroid cancer progression. In addition to Vanderbilt Health, researchers from Johns Hopkins Medicine, MD Anderson Cancer Center and the University of Washington School of Medicine contributed to the paper.
“This type of study is groundbreaking in the field and wouldn’t have been possible without the fantastic coordination of multiple centers,” said Weiss. “And within our team at Vanderbilt Health, collaboration between pathologists, endocrinologists, oncologists, surgeons and bioinformaticians was paramount to support this work.”
Matthew Loberg, PhD, a physician-scientist trainee in the Weiss Lab, was the study’s lead author, and eleven other Vanderbilt-affiliated trainees contributed to the research.
In thyroid cancer, indolent tumors, or those that usually respond well to standard treatment, can progress to become aggressive. The study created one of the first large thyroid cancer single-cell sequencing atlases made up of cells from 81 patient samples, spanning both indolent and aggressive variants. It also leveraged a unique cohort of patient samples with spatial transcriptomics, which uses spatially bar-coded genomic data, to assess stromal changes across spatial progression of tumors from indolent to aggressive. The researchers used multiplex immunofluorescence to spatially confirm protein expression of genes and location of cell subtypes.

“We can use single-cell sequencing to identify the genes being expressed on a tumor specimen and combine these data with spatial transcriptomics to see where those genes actually are,” said Ryan Belcher, MD, MPH, associate professor of Otolaryngology-Head and Neck Surgery and one of the study’s co-authors. “You can see the leading edges of invasion and recognize whether a cancer specimen has aggressive features.”
The study analyzed 28 spatial transcriptomic samples of thyroid cancer including rare anaplastic thyroid cancer tumors from adult patients, the most lethal type of thyroid cancer, as well as samples from pediatric papillary thyroid cancer. One of the next steps in the research will be to compare the information gathered from adults and translate it to understand the treatment of children who suffer from thyroid cancer.
“We want to understand better why pediatric patients end up presenting with more aggressive features such as lymph node and lung metastasis, and this type of study will help us understand that better,” said Belcher. “This type of research has been done with other tumors, such as breast or lung cancer, but it had never really been done with a large cohort of thyroid cancer patients. … To us, it’s a stamp of how important our research in pediatric and adult thyroid cancer is at Vanderbilt Health and at Monroe Carell Jr. Children’s Hospital at Vanderbilt as one of the leading institutes in thyroid cancer research in the country.”
Belcher added that while this research may not save a life tomorrow, the answers it seeks to provide in the long term can very much help families down the road.
“Thyroid cancer can recur, so there’s hope for the creation of drugs that can treat the cancers associated with CAFs,” he said. “And that may be an option for patients of any age whose thyroid cancer comes back, as well as any future family members who suffer from it.”
Weiss said that this study underscores how seriously Vanderbilt Health takes every facet of patient care, from the research that lays the foundation for future treatment to the moment it is administered to save a life.
“This paper was made possible by dozens of physician-scientists at Vanderbilt and beyond, each of whom plays an important role in working toward lifesaving care beyond just the operating room,” said Weiss. “Vanderbilt is known for its creative and collaborative culture. We make the biggest discoveries and advances when we work together as a team.”
“We’re not just here to do a patient’s surgery; we’re here to perform game-changing research because we care about this disease process and making it better,” added Belcher. “This is all we think about. It’s our passion.” This research was supported by the National Institutes of Health (grants R35GM122516, R01CA244188, R01CA272875, K12CA090625, K08CA240901, F30CA281125, T32GM007347, U01CA294527 and R01DK103831), American Society of Cytopathology, American Thyroid Association, V Foundation for Cancer Research, Children’s Cancer Research Fund, American Cancer Society, Petrick Thyroid Cancer Research Fund, Johns Hopkins Cancer Convergence Institute, and Sidney Kimmel Cancer Center at Johns Hopkins.






